So I managed to copy this onto a new post. I've still not seen the thrombosis /haematology doctors but apparently they are coming to see me today, where have I heard that before?! 🤔
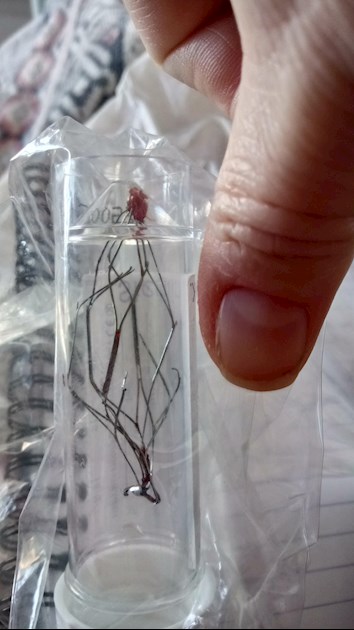
I have attached a photo of the filter with my thumb beside it to give you an idea of the size of it, the metal side struts had to be collapsed back through the vein, and apparently that is a piece of my vein wall still attached to the top of it😲!
"The filter is out but the surgeon had a major shock when he first imaged it, in fact he said it was the worse case of filter embedding, scarring and erosion he had ever seen. The entire filter, rather than being inside the inferior vena cava vein, had eroded through the vein wall so that the filter encased the vein!
I was in surgery for almost five hours and lost a fair amount of blood but he managed to avoid open surgery and to retrieve it via my veins using three puncture sites, my neck and both groins.
The entire top apex was encased in scar tissue and there was only one tiny hole in it where he was able to pass a guide wire through to get to the filter. All the returning blood from my lower abdomen and legs has had only that small hole in the scar tissue in which to return back to my heart. It's no wonder then that I have been so unwell and in such terrible abdominal pain since 2015 and then house bound for the past year and a half, with excessively high heart rates and acute breathlessness
Apparently my poor heart has been compensating for this lack of returning blood for many years, as the blood flow back up to my heart declined and worsened! With my sticky blood and delicate EDS connective tissues, it was a a disaster waiting to happen and should never have been put in, well not a permanent filter anyway.
My main abdominal vein has been left so scarred and narrowed that he had to insert a stent in it, in order to keep it open and post op I feel worse than I did before.
My lovely cardiac/respiratory doctor Dr Marino came to see me today and explained that it will take my heart some time to get used to the new increased blood flow and pressure and after having a listen to my lungs told me that I also have fluid on them due to being intubated, which is exacerbating my breathlessness and reducing my saturations. At the moment I'm on 24 hour oxygen to help keep my saturations up and to ease the pressure on my heart while it learns to adjust.
I almost didn't go ahead with the operation, as Dr Breen didn't come and see me on the ward the day before when I was admitted as promised and has yet to come and see me post op, which is incredibly disappointing.
It may not have been a her fault pre op, as the ward I was supposed to be admitted to had no beds available and so I was sent to the Simon Patient Lodge, the in hospital hotel instead of being on the ward.
I only went ahead with it because the interventional radiologist who was going to perform the operation convinced me that he was fully aware of my clotting history and as such would keep me on a heparin infusion throughout the operation. He also said that he would keep me on heparin injections post op, until I am seen by the thrombosis team.
He actually showed me the ultrasound images of my operation from start to finish and when I saw that the filter was outside my vein, I was utterly gobsmacked that he managed to get it out, given that he had to collapse it back inside the vein which would have punctured the entire circumferance of my vena cava! He said that he had to apply pressure on the vein for a very long time afterwards in order to stop the bleeding!
My haemoglobin pre op was 9.7 so anaemic and post op 7.4 so very anaemic, so far I've only had IV fluids but hopefully if I eventually see the thrombosis /haematology team, they will arrange for either a blood transfusion or iron infusion to rectify this.
It's been incredibly frightening going through this operation and recovery without the support of the thrombosis doctors, especially as I am feeling what is either blood clots or scar tissue debris passing through my heart and into my lungs, whenever I move around, say from bed to commode. I've also been having head and eye pain, zigzags and peripheral flashes and very blurred vision, in fact I have to say that l feel a bit like a ticking time bomb😮
Today my face was so flushed and burning it felt like I'd exposed myself to several hours in the sun. It is butterfly shaped on each cheek but not really on my nose, so I don't know if it can be considered as the classic lupus butterfly rash. If I can work out how, I might try and post a photo to see how it compares to other people's.
I might have to copy this post to a separate post tomorrow, as I'm not sure if this one is still being followed. Hope that I made sense above, as I don't really feel in charge of either my brain or body at the moment 😖. "