I’ve been on the forum for a few months after being diagnosed with Graves Disease on September after my health deteriorating significantly after giving birth to my first child in February.
I was bounced around the NHS system for months as they couldn’t work out what was going on with me until I reached 55kg, and my next door neighbour who’s fortunately my GP nurse stepped in and added Thyroid Function tests to my blood panel that they’d requested.
I’m currently under an endocrinologist at Royal Stoke but he’s already handed me off to a registrar after “significant improvement” who in turn decided that with my weight gain I was over medicated on Carbimazole , although feeling much better in myself.
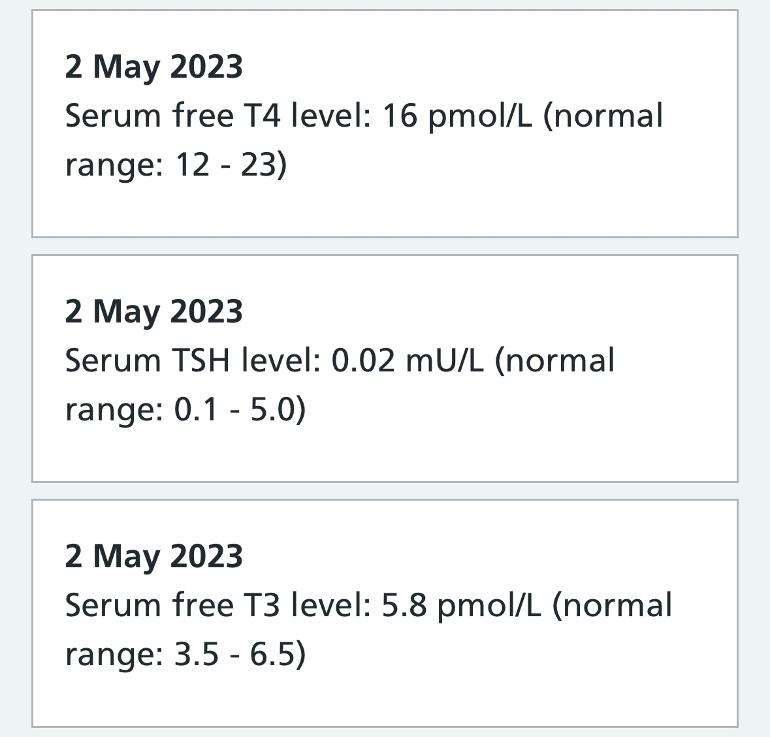
My recent bloods show as per attached with ranges. (I know I’m lucky to get them to test T4 & T3 but that’s with a lot of persuasion after being so “out of range”)
I’m booked for a telephone consultation with both the registrar on Wednesday and the GP on Thursday.
Does anyone have any recommendations on how to advocate for myself that feeling better in myself, a lot less anxiety even without my propranolol yet I’m always tired and now require 10 hours of sleep to be able to keep up with my 15 month old and work full time.
Thank you in advance