So I am so upset with the medical industry because they say well we did " a blood test on you ( only the ANA. ) And it came back negative, now this is just with a regular doctor who knows nothing about lupus. I do because my mother had it and she passed away from multiple organ failure which was her Lupus. She had it bad, and so do I. My mom's doctor's could never find hers either until eventually she had a mini-stroke at work, and then was diagnosed with lupus after running a 10 panel blood test on her just looking for autoimmune diseases. Now I'm trying to find a community that has lupus so you can look at these pictures and tell me what you think. This is a picture taken tonight while cooking dinner. It was 66 degrees in the house, and just a regular light on the kitchen. This is constant too! My face turns this maroon color too! But my legs here in the pic are covered so no redness. If I go outside Even for 5 minutes in the sun , I feel very sick, I'm red all over, and I start having a flare up. What do you all think this is? It's got to be lupus...what else could it be. ( My mom told me that ANA's can come back with a false positive) meaning I am really positive for lupus. I'm at a complete loss. Please help. So glad I found this website
If this isn't lupus, I don't know what is - LUPUS UK
If this isn't lupus, I don't know what is
Hi LupyJes, so sorry to hear about your troubles, both with illness and with the medical profession! There are plenty of people on this forum with doctor-related problems; in fact, it’s hard to have an autoimmune disease without doctor problems too! I’m not sure about your rash, I have a similar rash (though not to the same degree) and it’s only recently started happening for me, while I’ve had lupus for at least 15 years. So it’s worth remembering no 2 presentations of lupus are the same. Even though your mum had it, and even though you might have it, yours might look completely different to your mum’s. It’s part of the difficulty of finding the root cause of your symptoms.
Lots of doctors won’t consider lupus with a negative ANA, rightly or wrongly, so it’s hard to get a diagnosis if you don’t clear that hurdle. That said, it is possible to have seronegative lupus (lupus without the positive bloodwork). What you really need is a specialist—for lupus, this is usually a rheumatologist or immunologist—who is prepared to look beyond bloodwork and think outside the box with you.
In terms of your rash, there’s lots of things it could be. The most common rashes with lupus are the classic malar rash and disc-shaped rashes, but there’s heaps of others, and some rashes are completely unrelated to lupus. I have several comorbid illnesses, they exist alongside lupus, but are not necessarily caused by it. Although it could also be argued that having that inflammation in your body makes you more susceptible to other illnesses!
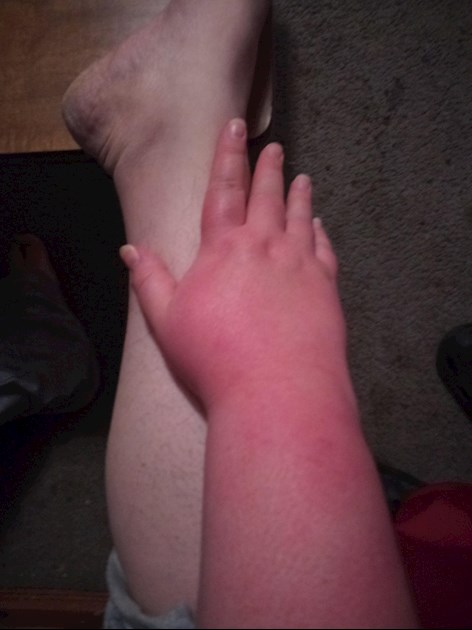
Your rash looks like maybe CRPS or Erythromalalgia, but you’d need to check their other symptoms alongside yours to see what matches. Good luck, and please do post here with any other questions or even just to vent. We know how this feels!
Hi Jes I am so very sorry that you are not having any joy with your Doctors. It is soul destroying and stressful when you are struggling and have no answers. I would ask for a referral to a doctor who specialises in Autoimmune conditions. I don’t think there is a typical Lupus rash, everyone is different but they normally have a sort of pattern and yours is just red and angry. It looks painful. Keep photos and a symptom diary and ask the question you have asked us, if not Lupus what is it? I am so very sorry to hear about your Mum. Keep us updated xx
I have also 💭 it could be Mitchell's disease... Is that what your talking about?
Thank you so much for the kind words as well about my mom, I am more than heartbroken over it.
You will be devastated. My mum died of severe atherosclerosis with unspecified autoimmune disease - likely Lupus but she was never tested nor even aware that she may have it. But it doesn’t mean you will have the same problems as her anymore than it means I’ll die of atherosclerosis or Diabetes like my dad. Try not to assume that what happened to your mum will inevitably be the same as what’s happening to you. X
Yours does have the appearance of Erythromelalgia - which I have myself. It’s not called Mitchell’s disease now because he had a rather dubious reputation as a neurologist who believed in women were suffering from hysteria and sent them to sanatoriums back in those days.
But yes that is what is now known as Erythromelalgia - which can be associated with many conditions, some genetic, some autoimmune and some malignant - or just idiopathic ie cause unknown. It is not specifically associated with Lupus - and is probably most closely associated with RA and Sjögren’s of this rheumatic disease family but also with MS.
Increasingly it’s thought to be the cutaneous manifestation of small fibre neuropathy and is a neurovascular disorder. Here are a couple of good links I’ve found helpful. I would try not to focus too much on ANA and Lupus just because it affected your mum. Autoimmune diseases can sometimes run in families but one person might have RA amd another might have Graves or MS or hypothyroidism.
Just keep an open mind but I would definitely research Erythromelagia.
sruk.co.uk/scleroderma/eryt...
I found these links very helpful for me, thank you!
I’m sorry to hear that you are suffering so…I ,for a time, was convinced that I had lupus too but the tests kept coming back relatively normal. I ended up sharing my story with someone who was diagnosed with Mast Cell Activation Syndrome.
It turns out I too have MCAS. It is a disorder that drs have little knowledge about and like lupus it presents in so many different organ systems with varying symptoms.
Your arm looks like mine so often did before treatment.
I see an allergist for treatment but immunologists are an even better bet for being informed.
I Hope you get to the bottom of this very soon and can find some healing methods.
There are so many autoimmune conditions that share symptoms (including photosensitivity) so I wouldn't want to even hazard a guess whether this was lupus or not. I, like your mum, also suffered a stroke, at 16 years old. I was diagnosed with systemic lupus but it was the Antiphospholipid syndrome that actually caused my stroke. In 27 years of being diagnosed with lupus (& all the other crap) I have only had a positive ANA about 3 times. The rheumy that diagnosed me was actually a lupus specialist & he himself told me that ANA is not a definite yes or no, it's PART of the criteria they use. People who are perfectly healthy, with no issues at all can have a positive ANA at times...it all depends on what's going on in your body. My ANA has also been negative when I've been in the middle of a massive lupus flare (just goes to show!) so once again, I repeat, the ANA is not a definite yes or no, despite what you are told. Read up on seronegative lupus openaccessjournals.com/arti...
Hi sher78, I’m waiting on a diagnosis of what actually is the matter with me, I’ve had flares for the past 15years, along with lots of other symptoms between flares, I’ve recently had a baby and they found I had kidney disease during pregnancy, I’ve had lots of Ana, anca, ro, sm, and igg acl antibody bloods tests and all have been negative, I also tested negative for ds dna specific for kidney disease.Has anyone had a lupus diagnosis with all antibody blood tests negative? I’m going around in circles and feeling so ill, and at present not taking any medication apart from amitrypline for migraine auras, it seems I’ve got most symptoms of lupus but blood work negative is it possible to still have lupus?
Thanks in advance for taking time to read the above
Stage lll or lv kidney disease gives ten points on the weighted point scale so it meets diagnostic criteria sans positive serum results.
My nephrologist has said he thinks I have iga n, he does not want to confirm by biopsy as they are stable at present and he said biopsies can aggravate, he’s said I’m early stages as kidney function etc is still normal and post pregnancy protein disappeared, is it only certain stage kidney disease that’s accepted for diagnosis of lupus?
It is very difficult to get an official diagnosis without serum positivity without severe organ involvement.
Thank you for replying, I’m just so unwell and have been for the past 5 months, I’ve had sun rash which is treated with steroids, and hair loss for 10 plus years, the past 4yrs I’ve suffered severe migraine plus auras, pain in joints and muscles and been diagnosed this past year with kidney disease, but never had positive blood work. All I really want is treatment as the pain is awful and I’m a mum again to a young baby and I’ve been a flare for the last 5 months, does it sound like lupus?
What serum tests have been run?
ANA 3 times, ANCA, ENA, ds-dna, cardiolipin igg, igm, la. All neg.Fbc- high platelets and mcv detected but b12 deficient so was told that’s why, all iron levels etc normal
Crp normal
Esr, high -29 but cut of is 20 so not seriously high apparently.
Also had lft, u&e, cancer screening, hormone and cortisol blood screen all normal.
Thanks for reading
Were APLs tested? Any history of miscarriage? I had life long migraine with visual aura and after having a PFO and atrial septal aneurysm fixed I feel so much better. After the heart procedure, diet and life style changes my apls and ANA and all other antibodies are now negative.
Yes all been tested and negative, 4 times since 2019. I’ve not had a miscarriage, and other blood tests with clotting etc been carried out, and been ok.So glad your feeling better and got reassuring blood tests, the migraines are awful but they come in flares, odd.
What I don’t understand is, it’s the auto antibodies that supposedly make you ill, isn’t it? so if you haven’t got them how can you have lupus, if they are what attacks your body 🤷♀️I’ve been reading a lot about sero negative lupus to make sense of it, but still can’t, hope you continue having good results and are healthy and happy in the future 😊
I feel better when my antibodies are not present. I have long remissions thankfully.
Generally speaking seronegative autoimmune diseases are thought to be milder/ less erosive versions which don’t cause much joint erosion or organ involvement. For instance I was diagnosed ten years ago with seronegative RA and put straight on methotrexate, which I took for a few years before I could no longer tolerate it.
I do have some left over ulnar drift from early days and I think it’s still active sometimes hence very high inflammatory markers when the pain returns - especially in my feet - my little toes are quite deformed now. So it’s done it’s thing slowly - especially since I couldn’t tolerate the main disease modifying drugs for RA and didn’t qualify for the next tier of anti TNFs or biologics.
Similarly my Sjögren’s is seronegative and hasn’t caused huge amounts of eye damage or mouth dryness or parotid damage - although my eyes are plugged and I use drops regularly, salivary stimulants and take the largest dose of Mycophenolate now to prevent further kidney damage or lung dabge from Sjögren’s and to get my immunoglobulins in range.
I do have severe small fibre and autonomic neuropathy though and Raynaud’s plus Erythromelagia and bad Gastroparesis and bowel damage.
But what I think still hasn’t been well understood yet at all is that seronegative rheumatic diseases are likely to form a unique subset of their own.
So in a sense it’s the labels such as Lupus and Sjögren’s and RA that are the problem here.
For instance psoriatic arthritis and ankylosing Spondyloarthritis aren’t always mild or non erosive at all but have a genetic component and are classed as autoimflammatory rather than autoimmine. And they don’t carry antibodies, they carry genes, so are inherently seronegative. And there is some thought amongst leading scientists now that seronegative Sjögren’s and possibly also RA and Lupus are part of this same autoimflammatory Spondyloarthritis family.
Which would make a lot of sense to me for people who have all the hallmarks of these diseases but not the ANA or ENA antibodies.
I’ve never been tested genetically at all and I think this is a real problem because Rheumatologists often don’t routinely test genes such as HLA b27 or less common and lesser known genetic markers. So the science hasn’t caught up and seronegative people fare worse in general because, as with my mild RA, it still creeps along unrecognised until irreversible damage occurs. I’m always being told I have irreversible damage these days 😢😡
And I say this as someone who has a kind of MCTD but with a highly specific scleroderma antibody which only showed up as my GI system started to fail a few years ago. I do have +ANA with an uncommon pattern for Scleroderma too . My former rheumatolgist won’t diagnose scleroderma despite being seropositve due to lack of skin thickening but says he thinks it’s my own unique Sjögren’s or Lupus antibody instead as it’s too rare to say and has apparently been found in a few with Lupus and UCTD. But 97% who carry it have systemic sclerosis.
I’m also hypothyroid which is usually autoimmune and I do carry the antibody but it’s only been moderately positive because it’s pretty well controlled with thyroid replacement now. But when it wasn’t my ANA showed high whereas these days it’s settled at a weak positive of 1:80.
So it’s all more complicated than just seronegative and seropositive or Lupus versus RA versus Sjögren’s or Vasculitis or UCTD or MCTD.
And often people who aren’t seronegative get diagnosed far too late for the disease modifiers to help so actually are worse off than seropositve.
And good rheumatolgists and researchers are very aware of this but are too overwhelmed by heaving clinic lists to be actively involved in research into seronegative rheumatic diseases.
Maybe more will emerge from the pandemic about antibodies and immunology but personally I think it is geneticists and the genome project that we need to get back to focussing on now probably. And there is hope that the OCTAVE study will emerge with very good new information about all this - because one of the leading professors involved is an authority on seronegative autoimflammatory diseases - particularly PsA. I’m pinning quite a lot of hope on this guy: gla.ac.uk/researchinstitute...
That’s really interesting thank you for responding, how easy is it to get a genes blood test? I’m going to see a rheumatologist in November privately, as I just can’t live like this without any treatment, it’s torture.I also have suffered with Raynauds for years, my mum has raynauds, sudden rashes but very occasionally, aches and pains, and we both suffer with a red nose rather than the typical butterfly rash.
There are so many more symptoms I have dry eyes, mouth, rash in any causes of heat not just sun but they appear different, I get hives in the sun that lasts until I take steroids. I had my baby 7 months ago and weigh less now than before pregnancy, I’ve no appetite, feel anxious and depressed, something I’ve never been diagnosed or treated for.
My skin hurts to touch in places, my vision has also changed dramatically, I had ct brain scan two weeks ago as had TIA symptoms but all was clear, I just don’t know what to do with regards to having any form of relief, all I take is paracetamol as I have kidney disease I can’t take anti inflammatory medicine and it doesn’t really do anything, thanks for replying 😊
Sorry I have no idea how you’d get genetic testing but I imagine most private clinics would be able to run these for you at a cost.
You could ask your GP first perhaps?
As others here have said your symptoms may well be part of a seronegative autoimmune or auto inflammatory disease - not necessarily Lupus though.
Sjögren’s and Vasculitis can both cause CKD and facial rashes too. I have early stage kidney disease from my Sjögren’s/ Overlap CTD. It’s kept in check but high dose of Losartan and mycophenolate.
I also have severe neuro GI motility problems relating to systemic sclerosis and had horrible post gestational facial rashes, allergies and alopecia.
It transpired to be Hashimoto’s hypothyroid disease and Sjögren’s - but I think I also have lots of other autoimmune and autoimflammatory diseases overlapping.
People, me included, tend to focus on one just disease we have heard of where it might well be other less well known or understood conditions. We can easily sort of make our symptoms fit the condition we have decided on without even realising that’s what we are doing.
For instance I was determined I didn’t have RA when it arrived in sudden onset ten years ago - but with hindsight I think I do have mild RA in my mix. Equally I decided that I certainly had Raynaud’s and Sjögren’s probably secondary to Lupus. WelI I definitely do have Sjogrens and secondary Raynaud’s - but, from my antibody and severity of my GI problems it’s more likely to be scleroderma related than Lupus - although I think I maybe do have some Lupus symptoms and signs in my mix as well including the facial rashes and neurological response to fleurescant lighting.
Then again this could be due to my histologically confirmed Sjögren’s?! 🤷🏻♀️
It’s all very confusing isn’t it, I just can’t go on living like I am, I just want to feel better, I hope that something can be confirmed so I can atleast treat it, the only blood tests I don’t think I’ve had is the c4 and c3 complement tests, is a reduce number in those part of diagnostic criteria? I hope your well and your illness is managed well, thank you for all the info it’s helped😊 it so lonely not knowing why you feel so ill, and the front you have to put on is so tiring 😫
You’re at the worst stage - I always say that psychologically being in the diagnostic wilderness while feeling lousy is far worse than even a bad diagnosis.
My Overlap syndrome is too complex and has been too misdiagnosed and untreated for too long to be well managed unfortunately. And I still don’t have enough clarity about which process is causing what, which problems are damage done and which are active disease. But I am now an acquired pushy bu**er so things are being clarified - not good news - but I always feel better for knowing what’s wrong for sure. I’ve never been able to play ostrich as some do - not many of us here can but definitely some people would rather not know.
My husband’s a bit like that so maybe a man thing and the majority here are women. But for me knowledge is power.
So best of luck and always prep for the worst case scenario - that of not knowing.
Rheumatology is the polar opposite of a black and white specialism and you may need to keep pushing on until you find someone who can think outside of the box. This way way you’ll hopefully not be too disappointed. Arm yourself with short list of symptoms and questions and yes get your compliments done by your GP or privately. Mine are weird as they are raised not low. Most with autoimmune diseases are low. X
Thank you, it literally sends you around the twist, it would be something if you could take something to relieve symptoms so you could actually enjoy doing anything with the kids, at the moment it’s living hell.Will definitely take your advice, thank you so much, I’ve seen so many different specialists over the years and it always comes back to autoimmune but then seronegative. Will take everything I can to rheumatologist and hopefully get somewhere, I’m definitely not a head burrier either, it’s impossible when you feel the way we do! 🤞 good luck with everything. I’ve appreciated all the responses you’ve given, I’ll also ask for complements test 🙂
I have had sero-negative Lupus for over 30 years. I was relatively lucky in that I initially tested positive but for the last 30 years I have been sero-negative. I was also extremely lucky in that I came under the care of a rheumatologist who recognised sero-negative Lupus, and they can be hard to find! I do not have kidney involvement. He is now retired but as you said you are seeing a rheumatologist privately I thought I would mention that all the rheumatologists at the Lupus Unit at the London Bridge Hospital trained under him and I would expect they would have a similar approach to sero-negative Lupus. Good luck.
The problem is unless there is a DEFINITE marker for a specific autoimmune, it can be an absolute nightmare to get a diagnosis. Many people are diagnosed with lupus-like conditions such as Undifferentiated Mixed Connective Tissue Disease. I guess it all depends on what your rheumy is like as like another poster has stated, trying to get a diagnosis without ANY positive lab tests at all, at any time... Just a thought, has anyone looked into the possibility of Ehlers-Danlos? I have recently been diagnosed with hypermobility EDS and was quite shocked at the similarity between the symptoms & problems caused by this & lupus, Raynaud's, Sjogren's etc.
There are many diseases that could cause such rash. Please keep digging and investigating with doctors to get to the bottom of it. Rheumatologist, dermatologist, immunologist - get everyones opinion until you get a diagnosis.
Hi there
Being ill and trying to coordinate your care including finding a medical professional that is willing to listen (as in, not listen to just respond but to listen and understand) is so distressing. So, combined with your family medical history, you're probably feeling soul destroyed, frightened and helpless.
I was in a similar position. However, my blood results were ignored until a diligent and wonderful Dermatologist identified them and carried out further tests and wrote a letter on my behalf. It was lupus and a few months later, something else and then... Sadly, the list grew.
However, 10 years previous to my lupus diagnosis, a rash presented in a very unusual and painful way. In a nutshell, it wasn't lupus but a very rare autoimmune condition that would not have been captured via an ANA test or any standard lupus blood tests. I had to attend a special testing unit to get a diagnosis. To date, I am regarded as being 'complicated' because I now have a multitude of AIs. Some common, some rare. Apparently, I'm susceptible to AI conditions.
What I'm trying to say is, and I know it must be very difficult, but try and let your specialists come to their own conclusions with, of course, the aid of your findings. As you don't want them to exclude/miss anything. I would strongly advise you to make detailed notes about your symptoms, when they happen, what time of day, photos, does it happen during your cycle, does it happen under certain lighting, do you get a rash? If so, does it weep? Are there any boils? If so, describe them and take photos. Do you get joint pain? Do your joints become inflamed?Also, on a separate page, include the symptoms of your mother as well. If you have a copy of her hospital letters, they would also be more than acceptable.
Keep everything factual. As in, evidence everything and don't forget to include the dates as well. Oh, and I know I'm repeating myself, but they love a photograph. Once you've collated everything, take it with you to your appointment(s). I presented mine in a folder. Yes, I meant business and in the end, they had no choice but to listen and take appropriate action!
Also, is there a medical professional that actually listens to you? If so, show them your findings and get them to write on your behalf to the other professionals involved in your case. Specialists are more likely to listen to a fellow medical specialist. They would never ignore them because it's a very small world and one day they might end up working with them or for them!
You CAN do this and don't give up hope!
Hey everyone thank you all so much for all this information! It's so nice to know that there are people out there who share in my stress, and wanting answers. Yes I do have the Molar rash or butterfly rash. Yes I do have photosensitivity, I cannot be in the heat or the sun. I will get a rash a couple of minutes of being in the sun or even heat. My face always has the " butterfly" rash unless I'm in my room laying in bed under my air conditioner. I had to put in my own air conditioner in my window because everyone else says it's too cold for them, but I live in my room in my bed with my air on constant and it's about 60 degree's in here, so if I'm not stressed or in the heat or sun I can keep my rash on my face at Bay, not always but alot better than if I'm outside. I also have more than just a rash or rashes, I have horrible inflammation, Joint and muscle pain, numbness and tingling in my extremities, fatigue, horrible pain in my legs, ( my legs ache all the time). So many symptoms. One doctor said I did have a positive ANA, and then she retired. Since then I've been tested with the ANA but it came back negative, so they said I didn't have lupus, Because there was no way to test negative on a ANA and have lupus. So why did my mom go with a negative ANA for over 10 years? Her eye doctor is the one who said she definitely had lupus and that's what caused her mini stroke to her eye and her left eye lost it's sight, also she had the dry eyes syndrome I can't remember the name of that, but it was called something. My grandfather passed away with what's called Good pastures disease, it is extremely rare and only 10 percent of men get this. It was caused from " untreated lupus" he went to the hospital and they said he had lupus for probably many many years and by the time he fell ill, his disease had went from this to that. Good pastures... It was awful! I know alot about lupus from my family history, and I don't believe that one ANA test can simply say I don't have it. Maybe I wasn't having a flare up at the time. Some people say that you should get a blood test done while your having a flare up. I wish I just knew because I feel horrible and if it's not lupus , then it really scares me that I have all these things wrong but no answers. I have heard I may have a rare disease called Mitchell's disease. I think someone mentioned that up above. I really appreciate all of your help, you all are so nice! Do you guys have to stay cool? Are you allergic to heat as well as the sun? Like if your inside and get hot do you have a reaction? I hate living in a dim lighted cold room but at least I feel the best like this. Also the humidity makes me feel really sick too!? Anyone experience that? I'm so sorry you all have to live with this awful disease. So many people don't know about lupus, or when you tell them that you're sick with lupus they don't understand that it's a real illness. If I say I had cancer everybody would know how bad I feel, but when I say it's lupus, it's almost like no big deal, it's all in her head. My mama called it the silent killer, and it's just so sad there's not enough support out there for people who suffer with this. You guys are wonderful by the way! So much 💕
I think you are focusing too much on Lupus. 30% of those with Sjögren’s are seronegative and also have similar mortality risks to those with Lupus - it’s an equally serious systemic autoimmune disease in its own right. Lupus isn’t an umbrella term nor is it worse than others of this family - it’s just all part of an autoimmune and autoimflammatory spectrum. If you’re able to get genetic testing this might help. Best of luck and please research Erythromelagia because to me your photo looks fairly classic of this rather than Lupus.
Hi Katy. I think you and I have a lot In common. Although I’m 64. I’m not going to give you my history here as there are so many above and the information is vitalBut gets confusing. I see a new neurologist
In December. I’ve developed what I think is EM/ what everyone is talking about. My skin doesn’t stay beet red and hot all the time but I feel it burning on low. Without my lupus meds it would be awful like you feel. When I have flares my hands, feet,
Arms, legs, face, neck, scalp are red and on fire. I’ve also read that there are other diseases similar. I’m hoping for a quick diagnosis yet accurate if there is such a thing lol. I’m in the US. Things get done faster but I’m hoping like you get relief. I live in a cold house. Air conditioner in our bedroom etc all things you mentioned. Good luck to us both. You are not alone.
Titters.