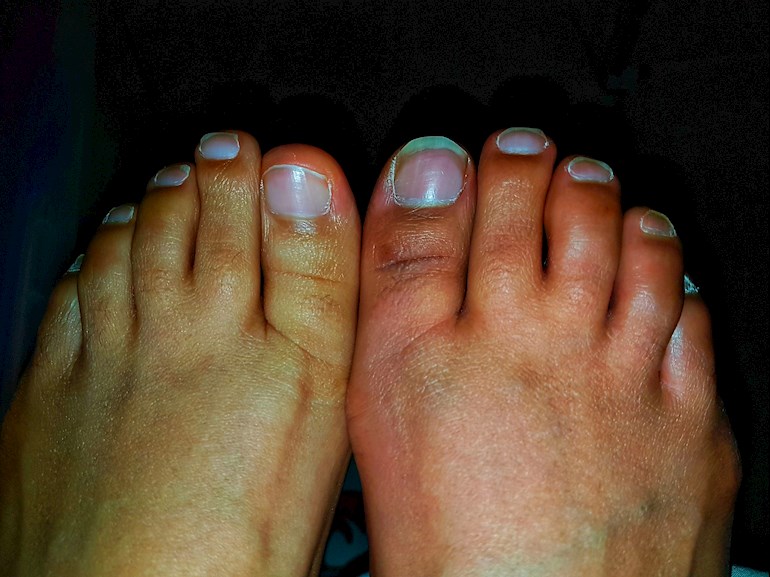
More frequently I am experiencing severe burning pain in my feet and lower legs. I have neuropathy in my feet and my Raynauds symptoms have been worse in the cold weather. This seems to happen over the course of a day. I often experience numbness in my feet but at the onset of these particular episodes, my feet will remain numb, I have difficulty walking as I can't feel my toes and they refuse to warm up over an entire day. Late in the evening, I start to feel a burning sensation and my feet will turn the same colour as in the picture, spreading from one foot to the other. My toes swell and become tight and shiny. Both feet and legs up to calf level feel as if I have poured boiling water on them or walked barefoot into nettles 😲. Gabapentin, Zapain and ibuprofen together do not help. Taking all three plus rubbing 5% ibuprofen gel on my feet offers some relief. I try to keep pain meds to a minimum so it really has to hurt before I up the meds. I generally don't sleep on those nights, so I am not good the next day. The one good thing is that these episodes eclipse all of the other aches and pains! I had an episode 2 days ago and still couldn't put weight on my toes when I went out today - relied heavily on my walking stick. I am seeing the consultant next week and hope that she will have some ideas. I just wondered if anyone else has this problem?
Ouch! Painful feet and legs - any ideas? Is this ... - LUPUS UK
Ouch! Painful feet and legs - any ideas? Is this part of lupus or something else?
Raynauds, by definition almost, is going to be worse in the cold weather. "Raynaud's disease causes some areas of your body — such as your fingers and toes — to feel numb and cold in response to cold temperatures or stress. In Raynaud's disease, smaller arteries that supply blood to your skin narrow, limiting blood circulation to affected areas (vasospasm)." This means it is important to wrap up warmly - and maintaining core temperature is just as important so body warmers usually help keep limbs better supplied with blood and warmer. You can get battery-powered boots and shoes as well - it is very important to keep your feet and legs warm. I know of one patient who moved house from the north to the south of England just because of her Raynauds. Another moved to Spain - and was finally able to wear a skirt in the summer!
It is difficult to know if your burning sensation is the reactive hyperaemia that often occurs after a Raynaud's vasospasm: the vasospasm can be so severe the tissue gets too little oxygen, a state called ischaemia, and then suddenly the toxins that are created lead to a short lived dilation of the blood vessels and loads of blood arriving to clear them out. That can be VERY painful. Or it could be another condition - which others on this forum know more about.
Thanks PMRpro for the comprehensive information, as always spot on.
My household nickname is Queen Manylayers ☺ I make it my business to stay as warm as possible and always have a bag of spare clothing/socks in the car when we're out and about. I usually wear several pairs of tights and socks and stuff the toes of those with soft toy filler which usually works beautifully. Heat pads and hot water bottles are my best friends. I also live in a warmer part of the UK. I have lived with Raynaud's for a while now and am used to the way my body responds to heat and cold so am querying this as it is quite different. I think that my worry is that this is another issue that is causing problems with my feet and affecting my mobility. I have a back injury that has affected my right leg and causes numbness in my toes, peripheral neuropathy which also causes numbness, Raynaud's which causes periodic issues, and now this. Lupus is just the cherry on top 🍒
Walking in the countryside and by the coast has always been a real pleasure of mine and a stress reliever. This is becoming increasingly difficult and I have been worried for a while about the consequenses of vascular insufficiency and tissue death. Sorry if I sound a bit ranty and sorry for myself.
Hardly - given the potential effects of both poor vascular perfusion and neuropathy it is hardly surprising if you need a bit of a rant!
It does sound as if there is some neuropathy going on there though doesn't it? I did wonder about whether maybe your several layers of tights/socks is making things worse - tightness isn't a good move.
Someone on a PMR forum some years ago said he had bought himself an "offroad mobility scooter" - he had refused to consider it for a long time as it felt it was a failure but having bitten the bullet he was able to get back to his favourite pasttime of walking the cliffs above the sea.
I suffer from the same and found 5 days of Iloprost infusions did help. They are not the most pleasant thing and unfortunately in this very cold weather the effects have been short lived.
Thanks Bronagh2015, it's good to hear that the infusions helped with your pain - such a shame that the effects werent longer lasting. Was that five consecutive days of treatment? That's a lot of time in hospital - I hope that you're keeping warm and well xx
Hello flap7
In line with what PMRpro says, I find that the Raynauds in my feet is more troublesome some time after the "blue" phase, and after my feet are warming. They usually ache intensely for a couple of hours and individual toes often turn pink/red (like your foot here) and painful at the same time. Although it's not obvious in my feet, I do get that tight and shiny look in my hands.
I find that the only solution is not to get cold in the first place - once it starts, I just have to grin and bear it. Unfortunately, on a typical day indoors, I often overlook the gradual onset of a Raynaud's episode in my feet until it's too late!
I don't know if that *is* what is going on for you - for example, your redness is more extensive than mine, but hope that helps. x
Thanks for replying whisperit, I'm truly sorry that you experience that whole horrible/tiresome cycle that comes with cooling and reheating. What you describe sounds terribly painful. It makes me appreciate even more the care and gentle humour that I see in your responses to others in distress. I absolutely get where you're coming from with the day to day management and sometimes catching it too late. Being vigilant all the time is exhausting - we need to be able to get on with our lives but balancing everything makes me wish for more hours in a day and a sheep/alpaca for extra wool! It has taken me two (3?) days to get around to responding to your post as I'm trying to get ready for seeing my first clients at my home next week. Loads to do but being unable to put either foot down properly without swearing luxuriously makes cleaning house/garden a slow process. Interesting for anyone in close proximity though 😂.
hello flap, just looking at your photo & reading your post & replies hurts...i am truly feeling your pain...and my feet & legs look just like your photo (my right leg/foot suffers more extremely from the red phase of my daily 24/7 freezing/burning cycle). My hands & head also suffer with the same freezing/burning symptoms cycle...so all my extremities are involved: it’s not a fun party!
My SLE was infant onset and i have the usual collection of comorbidities including early onset small fibre neuropathy/peripheral neuropathy + small vessel vasculitis + sjogrens...and my daily 24/7 freezing/burning cycle is diagnosed with early onset raynauds simultaneous with erythromelalgia & also in my worst forefoot i have CRPS (complex regional pain syndrome...which has a lot in common with erythromelalgia)
Here is a link to the most official & comprehensive info i’ve found on erythromelalgia (you’ll find lupus & peripheral neuropathy in the Related Disorders section...and, of course raynauds is covered too). This link is very good on diagnosis as well as both treatment options & self help techniques:
rarediseases.org/rare-disea...
Otherwise, have you posted your question on the HealthUnlocked Scleroderma & Raynauds UK (SRUK) forum? This forum has helped me a lot:
Rheumatology thinks i have systemic sclerosus in my mix of overlapping diagnoses, and my impression is that this can result in simultaneous Raynauds + erythromelagia....the SRUK website also has good info on erythromelalgia:
sruk.co.uk/scleroderma/eryt...
Hope something in there helps. Maybe you’ll ask your consultant about the possibilty you could be living with simultaneous raynauds & Erythromelalgia.... Erythromelalgia is considered a rare & unusual condition, and is not well understood by the medical fraternity...many consultants are not well informed about diagnosing & treating it...especially when it occurs simultaneous with raynauds, but, over the years, i have learned how to lifestyle manage this nightmare combination...and now rheumatology has me trying daily low dose losartan which will hopefully damp down both the raynauds & the erythromelalgia...my erythromelalgia burning flared terribly when i trialled daily nifedipine for my raynauds, which is why rheumatology is postponing a trial on IV illoprost
🍀🍀🍀🍀 coco
Coco, I really appreciate the time that you've taken to respond and I am gradually reading through all of the information that you have so kindly provided. Erythromelagia was one of the conditions that came up time and time again when looking for clues but I thought initially that maybe I was over-dramatising.
Funnily enough, I have visited NORD before looking for information, first when looking for information on symptomatic Tarlov Cysts then again when SLE became a possibility. The information for both resonated instantly for me and proved useful when explaining my symptoms to health professionals, ultimately resulting in proper diagnosis and appropriate treatment.
I honestly don't know how you cope with this 24/7 cycle - your courage and resiliance amaze me. I am coming to understand when it is happening and it seems to run 3-4 days just now, with a little respite before it begins again. With Raynaud's, the symptoms can be extremely painful but I manage to get a little sleep and can remain reasonably mobile and functional. This fire in my legs and feet seems to stop me in my tracks. I am also starting to feel the same stinging, burning sensation in my ear canals, of all the strange places.
I feel encouraged to ask my consultant to consider this as it is now really affecting how I function. I haven't cried once over the last year, despite the lupus diagnosis and back issues/ arthritis but I must admit, I did sit in bed on Friday morning and have a bit of a frightened sob about things. I am lucky to have a lovely supportive husband who does a great line in hugs and of course I have received a lovely virtual hug here, thank you ❤❤❤
Two quick questions, do you find that stress can bring about an attack for you and when your feet are red, are they hot to the touch?
Hello again flap...reading your wonderful reply, i just wanted to give you a virtual gentle hug...and next thing i read: there you were giving me one 😍!
Seems to me you’re doing ALL the right things...managing this is all about open communication with your medics + self awareness + trial & error...cause no 2 cases are identical and effective treatment plans take time to evolve
I should’ve mentioned that:
- i do think my daily combined therapy lupus meds do somewhat damp down the EM aspect of my daily freezing/burning RP/EM cycle (for lupus & co, i’m on hydroxy + myco + pred + amitrip).
- my rheumatologist agreed with me recently when i suggested science doesn’t really understand much about EM yet, but that my gut instinct is that EM is basically some aspect of RP gone 🤪 WONKY....she smiled and said: yes!
But certain triggers at max input do RELIABLY bring on my full scale EM attacks....at minimum input my EM still flares daily, but the redness, swelling, heat may be slightly less severe. These are CONSISTENTLY my main triggers (i’ve spent 15 flippin years studying this):
- physical activity, especially after midday
- time of day: my EM flares mostly afternoon into evening through till i get up in the morning
- warmer temperatures due to air, water, sunlight, heating, clothing (i go with skin exposed if poss, otherwise i mostly wear falke’s v lightest weight socks when i’m up and about because even when it’s cold around me any weightbearing activity will bring an EM flare on. When i’m sedentary, i need leg warmers, wooly socks + fleece booties...eg even in the EM flare part of my cycle, when i going to bed at night the deeper tissues of my feet & legs are freezing eith RP, so i need the layers in until the RP is overcome by the EM....i need to wear these layers all year round regardless of the season)
- lack of moisturing: i slather on shea butter twice daily...i think my need for this is due to overlapping issues (sjogrens + sclerosus especially)
- too much hard skin: every week i sand down hard skin around my heels where it accumulates most...if i don’t do this my EM feels a million times worse
You ask about stress: yes, stress “can” contribute to onset of EM-like signs & symptoms, but after years of building self awareness, stress isn’t one of my main consistent triggers..i think these EM-like s&s are more a reflection of my chronic dysautonomia + SLE neuro cerebral & small cell vasculitis manifestations than my EM/RP, although these all clearly overlap
I wanted to discover that certain types of food & drink consistently trigger greater degrees of EM severity, but 15 years of self- experimentation haven’t resulted in any consistent patterns of EM food reactivity
And, yes: when my feet/hands/head are red they are very hot to the touch, and swollen + shiny. Again, there is overlap here between, i think, my RP, EM, sclerosus and other stuff
😘🍀😘🍀😘🍀
Wow, oh wow!  I shouldn't feel excited over such a thing, but at last I'm not alone! I'm actually on this site due to heart problems, but back in 2009 I was really ill, and subsequently was told I had the antibody SCL70 indicating systemic sclerosis/scleroderma. For YEARS up to that point i had been suffering with what was eventually identified as erythromelalgia, but had been fobbed off by so many medics until other problems overtook me. I do have Raynauds but it is nowhere near as problematic as the Erythromelalgia, which had been hell to live with. I have photos identical to yours and plenty of other weird ones besides. I found that central heating worsened it (not the heat it created, just the type of heat). Having said that, excessive heat has always been intolerable for me and my symptoms, whereas excessive cold has been less so. Also, I couldn't sit or stand for any length of time without my feet becoming intolerably uncomfortable. They would improve massively with elevation. My hands were affected too, and again, elevation was the only thing to help. I'm using the past tense a lot, because, inexplicably after roughly 15-20 years of it, it abated massively, and even now I'm only getting the odd episode rather than it being a permanent state of affairs.
I shouldn't feel excited over such a thing, but at last I'm not alone! I'm actually on this site due to heart problems, but back in 2009 I was really ill, and subsequently was told I had the antibody SCL70 indicating systemic sclerosis/scleroderma. For YEARS up to that point i had been suffering with what was eventually identified as erythromelalgia, but had been fobbed off by so many medics until other problems overtook me. I do have Raynauds but it is nowhere near as problematic as the Erythromelalgia, which had been hell to live with. I have photos identical to yours and plenty of other weird ones besides. I found that central heating worsened it (not the heat it created, just the type of heat). Having said that, excessive heat has always been intolerable for me and my symptoms, whereas excessive cold has been less so. Also, I couldn't sit or stand for any length of time without my feet becoming intolerably uncomfortable. They would improve massively with elevation. My hands were affected too, and again, elevation was the only thing to help. I'm using the past tense a lot, because, inexplicably after roughly 15-20 years of it, it abated massively, and even now I'm only getting the odd episode rather than it being a permanent state of affairs.
I was initially referred to the Royal Free in London for the scleroderma side of things, but my diagnosis morphed into UCTD with elements of scleroderma, lupus and myositis (it turns out this is a good thing as it reduces the impact of the scleroderma). Iloprost infusions were discussed in relation to the erythromelalgia, but my symptoms improved to the degree where I felt I didn't need to explore further treatment. In all of my research over the years I have never come across anyone else suffering the same condition/s..
This probably doesn't help you much, I'm sorry, but when I get over the shock of finding not one, but two people with erythromelalgia, I may subsequently manage to come up with something useful 
Reward9, wow indeed! I am so grateful to you for sharing your story and am so glad that you are finally getting some respite from your erythromelagia symptoms after all these years. All of the information that you and Barnclown have so kindly responded with is enormously helpful - to hear that someone else has experienced the same symptoms is so important right now. I'm at a relatively early point on my journey towards diagnosis and treatment in commparison with many others here. Things seem to change from month to month for me at the moment so I wake up each day and just wait and see which new and exotic gift that lupus will present me with 🎁 It is interesting that both you and Barnclown have elements of sclerosis - so far I don't appear to have any markers for this but I know very little about it so it may be time to find out.
We have recently had heating installed that runs on an air to air heat pump so the dry warm air may be one of the triggers.
So glad you posted! 🏅🏅🏅
I get that too from time to time. My daughter also has Lupus and she was telling about her hot feet. So uncomfortable.
I have used this
Ketorolac Tromethamine 2% Topical Gel
It's a prescription and it helps.
Also same medication -toradol - Ketorolac Tromethamine - comes as a nose spray called Sprix if I am having a major bad joint day I use it. It has saved me from going to ER or using narcotics to mask the pain - best of luck