I live in the US - I have Aetna for health insurance. We specifically chose the highest plan my husbands employer offers, paying $800 a month (company matches half, so $1600 a month), for lower co-pays, lower deductibles, lower co-insurance.
I have an autoimmune disease, called Behcet’s. I have used my insurance A LOT. Multiple surgeries, hospital stays.
I recently had to stop taking Humira and start taking Remicade. Remicade is IV infusion, only.
When I went for my first infusion, I found out my hemoglobin was 5, so they had to start IV iron before I could start Remicade. Today was my 5th iron, and I’ve had 2 Remicade, my 3rd being due next week.
Now, due to co-insurance, I was told I would have to pay $266 per visit until I reached my $3000 for the year, and days I have both iron AND Remicaide, I double the payments.
Okay, fine. I can deal with that.
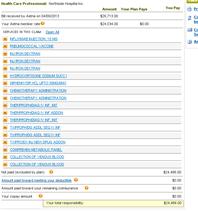
Then, I get an email today from Aetna. They denied my treatments.
I owe them $28 THOUSAND US DOLLARS FOR ONE TREATMENT. ONE!
Not to mention the second one I had that they haven't submitted yet!
I am so frustrated. I FINALLY find a medication that works, and then this. I am at the point of just giving up, crawling in a hole somewhere to die.