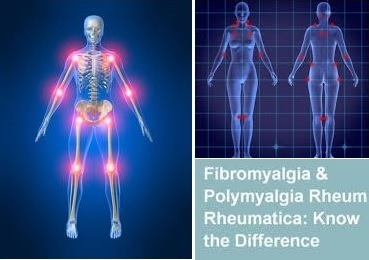
The differences between Polymyalgia Rheumatica (PMR) and Fibromyalgia (FM or FMS)
Polymyalgia Rheumatica is an inflammatory condition unlike Fibromyalgia which is not, it causes many painful muscles (poly = many, myalgia = muscle pain).
Fibromyalgia (Fibro = Fibrous Tissue it affects my = muscle algia =pain) is a widespread chronic pain and fatigue syndrome that is not inflammatory plus it is thought to possibly people may have a genetic predisposition to fibromyalgia.
FMS is reported to be Neurological with discussion of Central Sensitisation, please see link below for more information that may be of interest;
painscience.com/articles/ce...
In Polymyalgia Rheumatica (PMR) the muscles mainly affected are ones of the shoulder and thigh. The two conditions are similar as they often strike suddenly after a flu-like illness and the pain/stiffness is often widespread plus both feel fatigue and extreme tiredness.
Both PMR & FMS have no specific tests, but with PMR you may have blood tests to check for inflammation. However, inflammation ( ESR,PV,CRP) alone isn't enough to confirm a diagnosis of PMR as inflammation can occur in many other conditions, like infections and rheumatoid arthritis. Plus you could also be diagnosed with one condition that may or may not be of inflammatory cause and then be have secondary Fibromyalgia.
With PMR an ultrasound of the shoulders and hips may be used and can often show inflammation in the tissues and your healthcare professional may find tests show Anaemia (a lack of red blood cells) which is quite common in PMR, but you can be Anaemic in other conditions too. During or after a FMS diagnosis, bloods may also show a low Vitamin D or Vitamin B12, which may be treated with the relevant medication depending of the levels.
Steroid treatment can have a powerful effect in reducing inflammation in PMR but doesn't usually help in FMS long term. People with FMS taking steriods may have an initial feeling of improvement but it usually decreases after time. Steriods use in PMR won’t be a long term cure, they may improve symptoms significantly.
"Polymyalgia Rheumatica (PMR) is sometimes associated with painful inflammation of the arteries of the skull. This is called giant cell arteritis (GCA) or temporal arteritis and needs prompt treatment as there’s a risk of damage to the arteries of the eyes. About 20% of people with PMR also develop GCA, while 40–60% of people with GCA also have symptoms of PMR" (Arthritis Research UK)
Also Arthritis Research UK state that "Steroid tablets reduce the amount of calcium absorbed from the gut and increase calcium loss through the kidneys. To counteract this we recommend a daily intake of calcium of 1,000 milligrams (mg) or 1,500 mg if you’re over 60. A pint of milk a day, together with a reasonable amount of other foods that contain calcium, should be enough.
Vitamin D is needed for the body to absorb and process calcium. Your body produces vitamin D when the skin is exposed to sunlight. It’s also obtained from some foods, especially oily fish, and is added to some soya milks and vegetable margarines. It’s sometimes necessary to take a daily supplement containing 10–20 micrograms (μg) (this is the same as 400 to 800 international units (IU)) of vitamin D, especially for people over 60."
More information about Polymyalgia Rheumatica can be found here:
arthritisresearchuk.org/art...
and Fibromyalgia here;
arthritisresearchuk.org/art...
NB: All information based on my personal knowledge (from previous volunteering with the charity) of both these conditions therefore I am not a health professional so note that it is always best to consult your own Healthcare Professional. The information quoted in italics is from Arthritis Research UK and full information links to both conditions are given.
Hope this helps
AFMCG