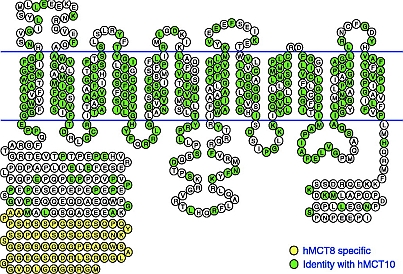
Another snippet of information about how the thyroid actually works.
My summary:
Iodine doesn't just hop into the thyroid as it passes in the blood stream - there is a special transporter mechanism that does the job.
If you have low/insufficient iodine, the transporter becomes more active.
If you then have sufficient iodine, the transporter becomes less active.
Chin Med J (Engl). 2014 Dec;127(23):4071-6.
Iodine deficiency up-regulates monocarboxylate transporter 8 expression of mouse thyroid gland.
Hu Z1, Zhuo X2, Shi Y2, Liu X2, Yuan J2, Li L2, Sun Y3.
Author information
Abstract
BACKGROUND:
Iodine deficiency is a major factor affecting thyroid auto-regulation, the quantity of iodine may greatly influence the synthesis of thyroid hormones (THs). It has long been believed that TH enters the cell through passive diffusion. Recent studies have suggested that several transporters could facilitate transportation of TH. The monocarboxylate transporter 8 (MCT8) was identified as a very active and specific TH transporter. The purpose of this study was to investigate whether iodine insufficient affected the expression of MCT8 in the thyroid gland.
METHODS:
Sixty BALB/c mice were randomly divided into two groups: control group was fed with standard feed (iodine concentration of 300 µg/kg); while low-iodine (LI) group received iodine-insufficient feed (iodine concentration of 20-40 µg/kg). After 3 months, 10 mice of each group were sacrificed. The remaining 20 mice of each group were kept till 6 months. From the LI group, we randomly selected 15 mice and injected triiodothyronine (T3, 100 µg/kg body weight per day) intraperitoneally for 24, 48 or 72 hours (5 mice for each time-point). Then, all the mice were sacrificed. Mouse serum thyroxine (T4), T3, and thyroid-stimulating hormone (TSH) levels were determined by chemiluminescence immunoassay (CIA). The protein content or messenger RNA (mRNA) level of thyroid MCT8 was measured by Western blotting analysis or real time RT-PCR respectively. MCT8 subcellular location in thyroid tissues was probed with immunohistochemistry (IHC) assay.
RESULTS:
We found that mouse serum T3 and T4 levels decreased and TSH level increased by the end of the third month. Consistent with these findings, there was significant goiter and hypothyroidism in the LI group. Meanwhile, the MCT8 mRNA increased to 1.36-fold of the level in the control group at the 3(rd) month. At 6(th) month, the serum T4 level in LI mice remained at a lower level, and MCT8 mRNA expression continued rising to nearly 1.60-fold compared with the control group. The protein content was also about 3 times higher than that in the control group. IHC results also revealed MCT8 was of higher expression and localized in the cytoplasm of thyroid follicular cells. After providing exogenous T3 to iodine deficient mice, the serum T3 and T4 gradually increased, whereas MCT8 mRNA and protein both started to decrease and returned to the same level as the control group.
CONCLUSION:
There is a compensatory increase in thyroid MCT8 expression to enhance its capability to transport TH from thyroid to the blood circulation in iodine deficient mice.
PMID:
25430451
[PubMed - in process]
ncbi.nlm.nih.gov/pubmed/254...
Earlier related article:
MCT8 transported issues are implicated in several disorders/syndromes:
rarediseases.org/rare-disea...
Rod