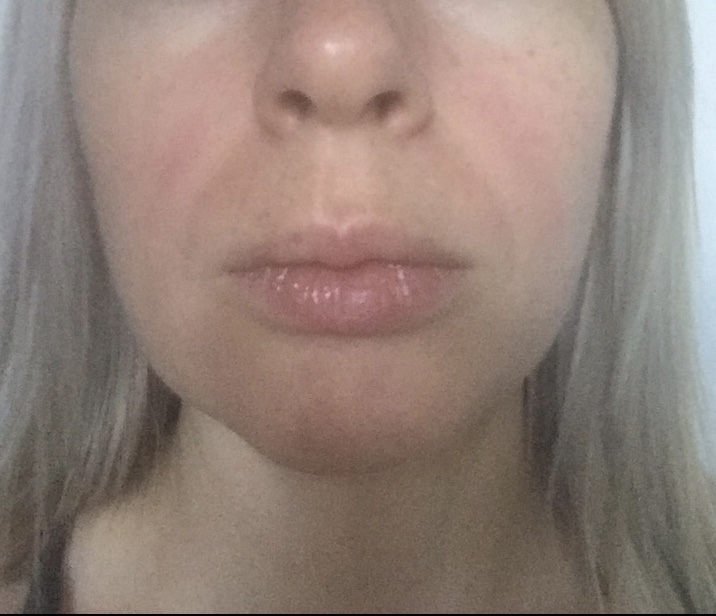
Fibromyalgia or Lupus? -( apologies awful photo quality my phone is ancient! Pic was a mild flare up, much brighter wen on holiday?)
Hi all, I’ve had an apt with a rheumatologist, she said straight away that I don’t have Lupus as my double strand test was negative. My ANA was positive but she said that it was ‘insignificant ‘ ?? My GP told me it was a lower end result 1:6 ?
And diagnosed Fibromyalgia.
I have almost all the symptoms of fibro however my only concern still is the rash on my face?
I get a red rash across my cheeks & nose when I’m exposed to sunlight? Within ten mins of being on a recent holiday my face was bright red, I explained to the doctor that it isn’t sunburn! It comes & goes.
I also suffer from recurrent kidney infection? ( 4 in 5 months)
Has anyone had similar experience pls as I don’t think my GP would be happy to refer me for 2nd opinion as they said the rheumatologist has final say? I understand that the double strand is negative however nobody can seem to answer why I get the rash? As this isn’t a fibromyalgia symptom?
Any advice greatly received thanks!