Hi
Other than a Chronic back pain and normal other conditions etc, I was feel for around 4 months off par, and then I had a very tender scalp, my eyes felt as if they needed wiping every hour or so, I had Jaw ache, and a headache but was not like a normal headache, my head was really not willing to cooperate with my demands, and generally felt lousy, so I decided to pay my GP a visit.
She checked with senior Partners and said she thought it was GCA.
I am getting a little anxious owing to the Diagnosis GCA not being confirmed after 7 months.
The GP thought it was GCA and immediately put me on 60 mg of Prednislone and next day I felt the best in years, however that soon vanisished and is a distant memory now. The GP sending me for two blood tests one of which was ESR. The following day my she the GP rang to tell me that the ESR test result was 86 (saying over 12 was high!)
My GP said he was treating my condition as GCA and still is, I went 4 days after initial diagnosis for a Temporial Biopsy proved to be negative, however after treatment for 4 days on 60 Mg Pred quite common to show negative, so I was informed.
The side effects are awful on the Preds, as I had a Flare after 3 months after reducing to 14 mg on original 60 Mg Preds, and was put back on to 80 Mg and side effects are really crippling me, I cannot do many things and sleep is virtually non existant, really feeling very low, I hope someone here has similar to me and can tell me how long I will need to recover from the preds, hope for positive news
Peter
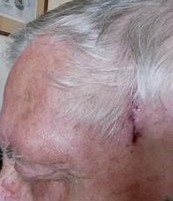
Picture after Biopsy, very quick and no pain then or after