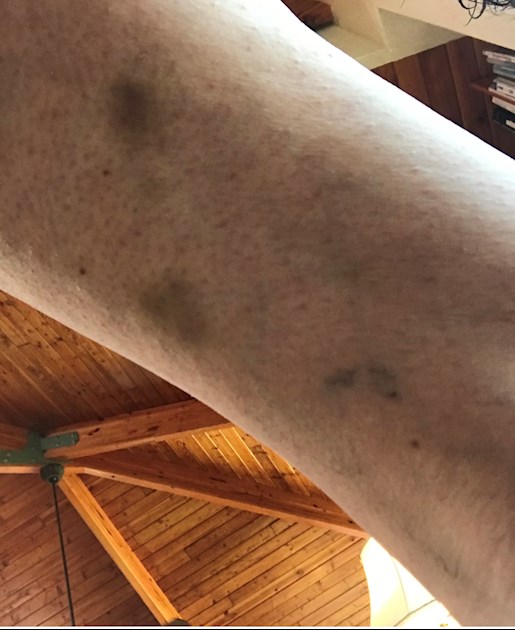
This is the back of my leg ( just above the bend of my knee ) yesterday. My arms are clotting also. When I clot, I tend to clot “ every where at once.” It’s like my body gets “ rushed “ with antibodies. I have not had any kind of dip in INR to cause this. My INR is set at about 4.0.
I am in 16.75 mg warfarin at the exact same time every night.
I eat the exact same amount of greens each day without fail. ( I follow the same line of thinking as cath Atkins. )
Nothing in my life , diet , no virus in system, etc... nothing can account for it.
It is my belief that our bodies go into APS “ flares” and when this happens we have antibodies “ rush “ our systems. I had posted this question some months ago trying to get fee back but not a lot of you seem to have this particular phenomenon with a rush of systemic clotting to all limbs. ( both arms, both legs, some organs- likely organs are MAPS- micro APS - micro clotting- very tiny and warfarin is handeling it fairly well compared to pre diagnosis and warfarin commencement.).
I keep clotting so it is once again considered “ therapy failure.”
I’ve failed before with DVT’s on warfarin alone, and was switched to LMWH exclusively- and got a DVT within less than a month- and symptoms far sooner. That did NOT work.
This has been a rough week.
Trying to save my eyesight, and possibly- distant future if we can’t get under control- limb. ( right arm, as Brachial has become quite narrowed with so many repeated DVT’s- always resolves, but at times can take up to 4 weeks- and superficial struggle to do a ,” work around.”
And brain is a concern- as my leg livedo can be quite classically pronounced, as I’ve posted a photo of once. ( livedo has been more closely associated with stroke tendency, but I’m unclear by what degree the risk factor increases.)
We are out of safe and reasonable options, I’m now told.
It’s very unsettling ( to say the VERY least) to go into uncharted waters with regards to anticoagulation ( new DOAC Meds) that did not meet RAPS trial .
Here is the Protocol/ Plan for me set forth:
l. Cytoxan (1000mg/m2) IV 60 every 4 weeks x 3 - so three months
II. THEN, after infusions- follow it with Either methotrexate 25mg PO ( then I can’t read his writing .. I think it’s more than once a day.. has 4 initial! I’ll post photo of his hand written instructions to me this in another photo... )
OR...
Imuran... 50 mg PO QD
And... concurrently, from day one, bring off the warfarin and I up the new DOAC. ( Xeralto or Eloquis WITH an anti platelet. )
——————————————————-
The idea is with suppression there will not be such a great need for thinning- well- yes there will be of course. Life long obviously. But hopefully it will make it “ safe” for me to be on a DOAC with anti platelet added as “ extra insurance coverage” against forming a clot.
Aggressively work on this from the auto immune stand point- for about 18 months I think. Then see how often we need to revisit that with the less aggressive oral drugs like Imuran or methotrexate.
Again, for those of you who have been through a similar treatment with any kind of actual suppression, or administration who can speak to because of your archiving of publications ( vetting of publications) talents, years of experience, and wisdom to be admin- I’m listening and needing your stories, guidance, advice. I’ll be making this decision ultimately.