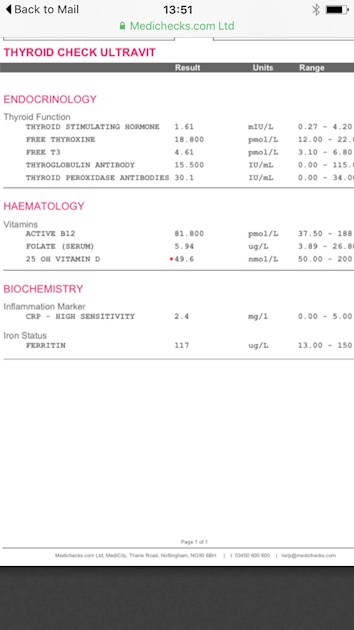
Hi I have attached my recent Medicheck Thyroid results. I have been taking 100mcg Levothroxine daily for 25 years. For all of this time I have felt emotionally dulled, no libido, waking several times in the early hours with muscular aches & pain, waking around 4am with a physical dump feeling. Recently I have mentally slowed down (age 62), I am waiting for results of my cortisol test. My freeT3 is mid range do you think I would benefit from T3?
Do I need T4/T3 combo : Hi I have attached my... - Thyroid UK
Do I need T4/T3 combo
Hi Fizzygig
do you think I would benefit from T3?
It's a bit difficult to say at the moment.
For thyroid hormone to work properly you need optimal nutrient levels and for good conversion of T4 to T3 to take place it's said that ferritin is recommended to be at least 70.
You have some issues with your results that ideally should be dealt with first before deciding to add T3.
Firstly, your TPO antibodies are so close to the limit at 30.1 (0.00-34.0) that I wouldn't be surprised if you have autoimmune thyroid disease aka Hashimoto's. Have you had antibodies tested before? Have they every been over range? Have you had fluctuations in symptoms and results?
Some people find that a gluten free diet helps reduce antibodies, also taking selenium l-selenomethionine 200mcg daily, the selenium helps with conversion of T4 to T3 too.
Vit D is way to low at 49.6nmol/L and this could be connected with your muscle aches and pains. The Vit D Council recommends a level of 125nmol/L
vitamindcouncil.org/for-hea...
so I would be looking at improving that by taking the amount of D3 recommended by the Vit D Council to raise your current level to the recommended level, ie 4,900iu daily (nearest available to buy is 5,000iu) and retest after 3 months. As it's possible that you have Hashi's, then an oral spray is best for absorption, eg BetterYou. They do 3,000iu and 1,000iu versions. I would start with the 3,000iu spray and take 6,000iu daily to start with.
Once you've reached the recommended level then you'll need a maintenance dose which may be 2000iu daily, maybe more or less, maybe less in summer than winter, it's trial and error so it's recommended to retest once or twice a year to keep within the recommended range. You can do this with a private fingerprick blood spot test with City Assays vitamindtest.org.uk/
There are important cofactors needed when taking D3 as recommended by the Vit D Council -
vitamindcouncil.org/about-v...
D3 aids absorption of calcium from food and K2-MK7 directs the calcium to bones and teeth where it is needed and away from arteries and soft tissues where it can be deposited and cause problems such as hardening of the arteries, kidney stones, etc.
D3 and K2 are fat soluble so should be taken with the fattiest meal of the day, D3 four hours away from thyroid meds.
Magnesium helps D3 to work. We need Magnesium so that the body utilises D3, it's required to convert Vit D into it's active form. So it's important we ensure we take magnesium when supplementing with D3.
Magnesium comes in different forms, check to see which would suit you best and as it's calming it's best taken in the evening, four hours away from thyroid meds
naturalnews.com/046401_magn...
Check out the other cofactors too.
Folate is low at 5.94 (3.89-26.8) and this should be at least half way through range. Folate rich foods will help, as will a good B Complex containing 400mcg methylfolate such as Thorne Basic B or Igennus Super B at the recommended dose.
Active B12: 81.8 (37.50-188.0) Opinion varies on this. One article recommends that anything below 70 should be tested for B12 deficiency. You don't come into that category but it is quite low and fairly close to that limit. You could check for signs of B12 deficiency here b12deficiency.info/signs-an... and if you have any then list them to discuss with your GP and don't start the B Complex until after further testing as the methylfolate contained in it will mask signs of B12 deficiency.
If you don't have any then you might want to consider a sublingual methylcobalamin lozenge. But the methylcobalamin in the B Complex recommended (400mcg) may be enough.
Ferritin is good.
I would suggest you work on your vitamins first, give it a few months and then repeat your test and see how your levels lie and how you feel.
Don't start supplements all at the same time, stagger them. Start with one, give it a week or two and if no adverse reaction then add in the second one, give it another week or two and if no reaction add in the next one, etc. By doing it this way, if you do have any reaction you will know what caused it.
Thanks for your comprehensive & very helpful reply.
I will check with my GP regarding previous TPO antibodies, this has never been mentioned before. Not sure which of my symptoms could be attributable to thyroid issues, menopause, stress or just getting older. The only information I have been given was that I was over suppressed for several years on 150mcg , this was reduced gradually to 100mcg by new GP about 4 yrs ago, didn't notice any changes in my health for better or worse.
Please excuse my lack of knowledge, not sure what the difference between hypothyroid & Hashimoto's is? Would it make any difference to my treatment if I did have Hasimoto's ?
I had already started supplementing with Selenium, & Zinc prior to my blood tests. I am going to phase in D3 as recommended, B complex with folate & magnesium over the next few weeks. I have also changed when & how I take my medication.
I have suffered with IBS since my early 20's well before my thyroid issues, I have never considered gluten intolerance as a cause, this has improved considerably with pre/probiotics use over the past 2 yrs. Do you think it is worth trying a gluten free diet?
Fizzygig
Hashimoto's is autoimmune thyroid disease, where antibodies are present The thyroid gland is gradually destroyed leading to hypothyroidism. There is no treatment for Hashi's, it's the hypothyroidism that it causes that is treated.
As you have IBS I would say it's worth giving a gluten free diet a go, give it a few months. If it helps, stick to it, if it doesn't then don't continue.
Thanks
I have just had my saliva cortisol result, they indicate phase 3 HPA (adrenal gland ) dysfunction & this explains a lot about how I feel. Now I am really worried about what this means for me. Can't get a GP appointment for 2 weeks & have lots of questions.
I have posted another general message on the site
Thanks
I was saddened to read your posting. Specifically, it troubles me to think that many days, months, and years have past throughout which you have felt unwell.
When you say that you have been medicated and suffering for 25 years, does this mean that you have never had a decrease or increase in your dosage during that time?
Why were you prescribed Levothyroxine in the first place?
I have a few ideas that might be supported or invalidated by your responses to these questions.
Hopefully, you are on your way to better living, with less discomfort!
Thanks for your reply .
Pre-diagnosis I suffered with extreme fatigue, muscle weakness thinning hair, brittle nails, unexplained weight gain, emotionally labile. Initially borderline hypothyroid - no treatment.
1 year later symptoms worse & now hypothyroid, referred to endo started on 25mcg gradually increased to 150 mcg & well over suppressed but much less fatigued & more emotionally stable.
On 150mcg for years but started to get chest pain (ECG OK) & benign arythmia. New GP reduced dose gradually to current dose of 100mcg , chest pain stopped, don't feel any different otherwise. Not depressed, tried antidepressants felt worse.
Now trying to understand my condition better gradually introducing nutritional supplements, pre/probiotics, change in the way I take my medication & doing more exercise. The worse symptom which never changes is poor quality sleep, no problem getting to sleep but very restless, waking in the early hour with an aching body & dumping/ flushing feeling in whole body. GP blamed menopause for symptoms , no better with HRT, well past menopause still no better. I know whatever time I go to sleep I will wake after 4 -5 hrs tossing & turning to get comfortable until it's time to get up for work.
Any insights or suggestions are welcome
Your vitamin D is terrible
Low vitamin D can badly affect sleep, and affect B vitamins
Getting vitamin D up around 100nmol is first step
Vitamin D mouth spray by Better You is good as avoids poor gut function.
It's trial and error what dose each person needs.
Once you Improve level, very likely you will need on going maintenance dose to keep it there.
Retesting twice yearly via vitamindtest.org.uk
Local CCG guidelines
clinox.info/clinical-suppor...
Government recommends everyone supplement October to April
gov.uk/government/news/phe-...
Also read up on importance of magnesium and vitamin K2 Mk7 supplements when taking vitamin D
betterbones.com/bone-nutrit...
articles.mercola.com/sites/...
healthy-holistic-living.com...
articles.mercola.com/sites/...
betterbones.com/bone-nutrit...
Do NOT supplement any vitamin K if you take any blood thinning medication including aspirin
drsinatra.com/vitamin-k2-su...
Vitamin C and bones
healthimpactnews.com/2018/d...
vitamin D is a pre-steroid pro-hormone, may be contributing to your low adrenal levels
Then look at improving folate by supplementing a good quality daily B complex one with folate in not folic acid
B vitamins best taken in the morning after breakfast
If you are taking vitamin B complex, or any supplements containing biotin, remember to stop these 3-5 days before any blood tests, as biotin can falsely affect test results
endo.confex.com/endo/2016en...
endocrinenews.endocrine.org...
Trying strictly gluten free diet is something to consider....perhaps in new year
According to Izabella Wentz the Thyroid Pharmacist approx 5% with Hashimoto's are coeliac, but over 80% find gluten free diet helps, sometimes significantly. Either due to direct gluten intolerance (no test available) or due to leaky gut and gluten causing molecular mimicry (see Amy Myers link)
Changing to a strictly gluten free diet may help reduce symptoms, help gut heal and slowly lower TPO antibodies
Ideally ask GP for coeliac blood test first
amymyersmd.com/2017/02/3-im...
chriskresser.com/the-gluten...
thyroidpharmacist.com/artic...
scdlifestyle.com/2014/08/th...
drknews.com/changing-your-d...
thyroidpharmacist.com/artic...
As SeasideSusie says....only add one supplement at a time and wait at least ten days to assess before adding another