Hello everyone, I've recently been told I have an underactive thyroid. I've been on 50mg of levothyroxine. I had no suspicion I had an underactive thyroid despite a strong family link, by blood samples were actually taken for other gastro concerns. I am feeling worse than ever; exhausted and breathless. GP not helpful. I have my blood results and was wondering whether anyone could offer any wisdom or insight as it would be appreciated! My GP left me out a prescription for thyroxine and that's been it. I'm a 28 year old female.
Newly diagnosed with underactive thyroid. Need ... - Thyroid UK
Newly diagnosed with underactive thyroid. Need help with blood results!
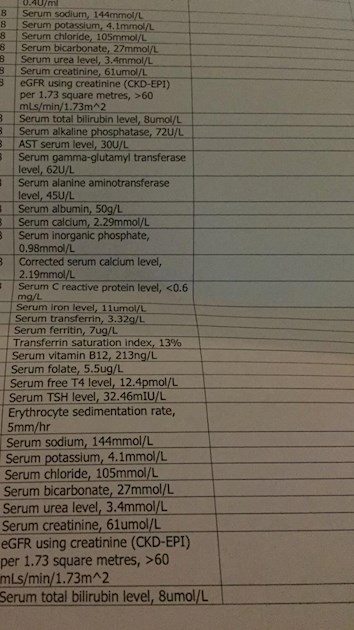
Oh dear - please could you add the ranges as labs do vary. How is your GP treating the LOW Ferritin & B12 ? Ferritin - stored iron - is seriously low - even without the range. Low Ferritin will cause fatigue and breathlessness. Without the ranges it is difficult to comment on your Iron Tests. Others will know more than me !
You will also need VitD tested as well as Thyroid anti-bodies TPO and Tg.
Ensure you are re-tested in 4/6 weeks to have your dose revised.
The above link takes you to the main website of this Forum where you can read all about the thyroid - testing - understanding results and so on.
To the right of your Post there are 10 more similar posts to yours - if your are on a PC. If you are on a phone then scroll down and down to view under Related Posts ....
Thanks so much for the reply Marz. This was the exact print out I was given with no ranges provided. My GP stated no concerns with any of my levels except TSH levels. I recently went to my GP surgery for a further blood test to check my thyroid antibodies and this was somehow lost! I spoke to another GP in the surgery who said it didn't matter anyway as we know I have an underactive thyroid so antibodies are irrelevant.
Sorry but anti-bodies are VERY relevant. 95% of Hashimotos sufferers are gluten sensitive - so they can be reduced by being gluten free. There is so much we can do to help ourselves. GP's do not know how to treat an auto-immune condition - so run a mile !
Are you in a position to do Private Testing though Thyroid UK - see link below and click onto ABOUT TESTING on the menu. It is the only way to find out the complete picture and for you to be well.
Also all the information on the website to learn about the thyroid and associated conditions. Information is power when it comes to having a meaningful discussion with your GP 
You are just diagnosed and must be feeling awful.
Levothyroxine doesn't work immediately. It takes about six weeks for the dose to be absorbed then you have blood tests every six weeks with a 25mcg increase until you feel much better and are symptom free. I will give you a list of clinical symptoms and you will be surprised you will have quite a few of them.
Levothyroxine should be taken first thing with one full glass of water and wait an hour before eating. Tablets could stick in your throat if not taken with sufficient water and food can interfere with the uptake of the hormones which you don't want.
When next blood test is due (I'd make an appointment on Monday well ahead) it has to be at the very earliest, fasting (you can drink water) and allow a gap of 24 hours between last dose of levo and the test and take it afterwards. This helps the TSH to be at its highest as it drops throughout the day and may mean you don't get an increase you need.
It is a big learning curve as many doctors don't seem to understand clinical symptoms or treat them but they mainly look at the TSH alone - which is from the pituitary gland.
Members cannot respond to your results unless the ranges are stated too (these figures are in brackets).
Your TSH is high and you will be feeling awful and the aim is to get it down to 1 (some doctors think when it is somewhere in the range (even top) that you're on sufficient but you need an increase.
You also need tested Vit D, iron, ferritin and folate. Always get a print-out of your results with the ranges. I note you have had B12 tested but the aim is a B12 of around 1,000.
thyroiduk.org.uk/tuk/about_...
pernicious-anaemia-society....
It is a big learning curve if we want to recover our health and be free of symptoms. If the doctor didn't test for thyroid antibodies, ask for these also. If you have antibodies you will have the commonest form of hypothyroidism - commonly called Hashimoto's (Proper name Autoimmune Thyroid Disease). Treatment is the same for hypo or hashi's. Going gluten-free can reduce the antibodies which attack the thyroid gland and wax and wane until we're hypo.
I am not medically qualified but if you can get the ranges of your results - put them on a new post for comments.
Thanks so much, that is really helpful! My GP give me a printout but with no ranges unfortunately. The antibodies blood test was somehow lost and GP feels this is not relevant anyway
Nothing seems to be relevant to doctors with anything thyroid. We have to read, learn and ask questions to recover our health to normal. Not be continually unwell because we aren't given thyroid hormones which suit us and relieves clinical symptoms.
I shall give you two links and people who have thyroid antibodies have an Autoimmune Thyroid Disease also called Hashimoto's for short. Antibodies can be reduced and helps prevent them attacking the gland until the person is hypo and will be hypo eventually but treatment is the same.
thyroiduk.org.uk/tuk/testin...
thyroiduk.org.uk/tuk/about_...
That's the reason we feel that antibodies should be tested so we can self-help to reduce the attacks ont he gland. Doctor thinks it is irrelevent as it is the same treatment, i.e. levo.
As has already been said, no ranges means we can't interpret your results. However, there are a few that are glaringly obvious even without the ranges.
Ferritin: 7
This is beyond dire. It is most certainly below range, most ranges start at around 13 or 15. Low ferritin can suggest iron deficiency anaemia. You now need a full blood count and if MCV is low with a high MCHC then that will confirm iron deficiency. Your other iron panel results don't look particularly good but difficult to say without ranges.
You will certainly need some supplementation and for a below range ferritin you should ask for an iron infusion which will raise your level within 24-48 hours, tablets will take many months. Once your level is up it can be maintained with tablets if necessary (or eating liver regularly).
For thyroid hormone to work (that's our own as well as replacement hormone) ferritin needs to be at least 70, preferably half way through range.
**
B12: 213
This is way too low. Check for signs of B12 deficiency here b12deficiency.info/signs-an... and if you have any make a list to discuss with your GP.
You really need testing for Pernicious anaemia and you may need B12 injections.
I have read (but not researched so don't have links) that BCSH, UKNEQAS and NICE guidelines recommend:
"In the presence of discordance between test results and strong clinical features of deficiency, treatment should not be delayed to avoid neurological impairment."
And an extract from the book, "Could it be B12?" by Sally M. Pacholok:
"We believe that the 'normal' serum B12 threshold needs to be raised from 200 pg/ml to at least 450 pg/ml because deficiencies begin to appear in the cerebrospinal fluid below 550".
"For brain and nervous system health and prevention of disease in older adults, serum B12 levels should be maintained near or above 1000 pg/ml."
**
Folate: 5.5
Very likely to be low in range although not sure if below range. If it is below range or borderline your GP should really prescribe folic acid but this must not be taken until further testing for B12 deficient/PA is carried out and B12 injecions/supplementation started.
SeasideSusie, thank you so much for taking the time to look at my results and reply. I know it's difficult without having the ranges. I'm concerned as to why my GP has not pointed out my low ferritin level nor provided a range. To be honest I'm really quite upset as these tests were carried out at the end of February and I've had no medication or supplements as a result. I've spoken to 3 GPs in my surgery regarding the breathlessness and none have pointed out my levels are low. I'm going to speak to them on Monday morning but I've feeling it will be a battle. I work full time and have young children and I barely have a moment as it is 😔
It is becoming increasingly common that we patients are having to do our own investigation and research.
I'm heartily sick of being fobbed off (an expression I used when speaking to my GP recently - he asked me what I meant!!! I thought doctors went to university and achieved degrees so should be well educated enough to know what fobbed off means!)
Apparently symptoms mean nothing, we imagine them or thinking about them makes them worse. Then they get ignored, no investigation and no treatment. I'm convinced I will die from something my surgery will ignore, and I doubt I'll be the first.
I'm thinking of asking for a refund of all my National Insurance Contributions that I paid over 46 years when I was working, and still pay tax which contributes to the NHS.
Stepping down off the soapbox now, it tends to get me a bit worked up 