I was on 75mcg Levothyroxine for a while after having Total Thyroidectomy last July, (came home on 100mcg Levo I believe ) had blood test and it was put down to 75mcg but just recently I have started to feel dreadful so went back to GP who agreed to put it up to 100mcg, don’t know if it was my imagination but next day started to feel slightly better and continued for a few days but yesterday 22nd May had a funny turn and felt sick and light headed, did not sleep well last night and feel dreadful again today, does this mean it’s the wrong dose still? I thought it was a bit quick to start to work but I’m now back to square one and I seem to be going to the loo a lot as in wee and💩 but not diarrhoea. The blood tests Iv put up are when I was on 75mcg and have to wait 6 weeks for new one on 100mcg to be done . Thanks for your input
Increase in dose of levothyroxine: I was on 75mcg... - Thyroid UK
Increase in dose of levothyroxine
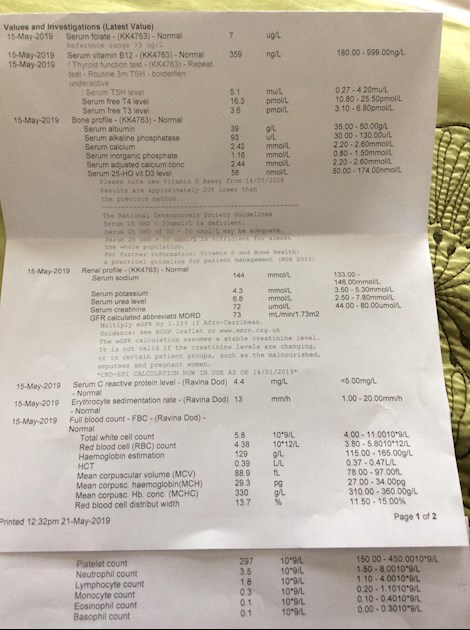
Results on 75mcg show you are very under medicated
TSH at 5.1 is above range
Bloods need retesting 6-8 weeks after each dose increase
For full Thyroid evaluation you need TSH, FT4 and FT3 plus both TPO and TG thyroid antibodies tested. Also extremely important to test vitamin D, folate, ferritin and B12
Low vitamin levels are extremely common, especially if under treated
Recommended on here that all thyroid blood tests should ideally be done as early as possible in morning and fasting.
This gives highest TSH, lowest FT4 and most consistent results. (Patient to patient tip, best not mentioned to GP or phlebotomist)
Last Levothyroxine dose should be 24 hours prior to test, (taking delayed dose immediately after blood draw).
Is this how you do your tests?
Private tests are available. Thousands on here forced to do this as NHS often refuses to test FT3 or antibodies or all vitamins
thyroiduk.org.uk/tuk/testin...
Medichecks Thyroid plus ultra vitamin or Blue Horizon Thyroid plus eleven are the most popular choice. DIY finger prick test or option to pay extra for private blood draw. Both companies often have special offers, Medichecks usually have offers on Thursdays, Blue Horizon its more random
Medichecks currently have an offer on until end of May - 20% off
Vitamin D definitely too low
GP will only prescribe to bring vitamin D up to 50nmol. Aiming to improve by self supplementing to at least 80nmol and around 100nmol may be better .
Once you Improve level, very likely you will need on going maintenance dose to keep it there.
Retesting twice yearly via vitamindtest.org.uk
Vitamin D mouth spray by Better You is good as avoids poor gut function.
It's trial and error what dose each person needs
Folate and B12 both likely too low
Supplementing a good quality daily vitamin B complex, one with folate in not folic acid may be beneficial.
chriskresser.com/folate-vs-...
B vitamins best taken in the morning after breakfast
Recommended brands on here are Igennus Super B complex. (Often only need one tablet per day, not two. Certainly only start with one tablet per day after breakfast. Retesting levels in 6-8 weeks ).
Or Jarrow B-right is popular choice, but is large capsule
If you are taking vitamin B complex, or any supplements containing biotin, remember to stop these 7 days before any blood tests, as biotin can falsely affect test results
endo.confex.com/endo/2016en...
endocrinenews.endocrine.org...
You need ferritin tested too
The aim of Levothyroxine is to increase the dose slowly in 25mcg steps upwards until TSH is under 2 (many need TSH under one) and FT4 in top third of range and FT3 at least half way in range
All four vitamins need to be regularly tested and frequently need supplementing to maintain optimal levels
NHS guidelines on Levothyroxine including that most patients need somewhere between 100mcg and 200mcg Levothyroxine.
Also what foods to avoid (note recommended to avoid calcium rich foods at least four hours away from Levo)
nhs.uk/medicines/levothyrox...
Official NHS guidelines saying TSH should be between 0.2 and 2.0 when on Levothyroxine
(Many of us need TSH nearer 0.2 than 2.0 to feel well)
See box
Thyroxine replacement in primary hypothyroidism
pathology.leedsth.nhs.uk/pa...
Dr Toft, past president of the British Thyroid Association and leading endocrinologist, states in Pulse Magazine,
"The appropriate dose of levothyroxine is that which restores euthyroidism and serum TSH to the lower part of the reference range - 0.2-0.5mU/l.
In this case, free thyroxine is likely to be in the upper part of its reference range or even slightly elevated – 18-22pmol/l.
Most patients will feel well in that circumstance. But some need a higher dose of levothyroxine to suppress serum TSH and then the serum-free T4 concentration will be elevated at around 24-28pmol/l.
This 'exogenous subclinical hyperthyroidism' is not dangerous as long as serum T3 is unequivocally normal
You can obtain a copy of the articles from Thyroid UK email print it and highlight question 6 to show your doctor please email Dionne at
tukadmin@thyroiduk.org
Professor Toft recent article saying, T3 may be necessary for many
rcpe.ac.uk/sites/default/fi...
Research shows 20% of patients after thyroidectomy can not regain full health on just Levothyroxine
ncbi.nlm.nih.gov/pmc/articl...
Thanks SlowDragon, folate is >3 mine is 7 so they may not request retest, others, ferritin, vit D and B12 say normal so I may have a problem requesting supplements on prescription. They weren't going to up my dosage because thyroid tests normal it’s only being on here and seeing information for others that I asked for 100mcg so thank you for all the information. I have to be re-tested in June when the calendars are fully up on GPS computers so I will as for all test to be done.
Forgot to mention that parathyroid was slightly high last time and it was redone but I have to wait til doc who ordered it comes back from holiday to interperate it. Receptionist told me that someone looked at it and said it’s fine no action but it has to be de iced by original requesting dr., so I’d like to see what the result is.
Vast majority of patients on here have to test FT3 and vitamins privately
You won't get a GP to prescribe any vitamins unless actually classed as deficient
So improving vitamin levels and retesting is down to you to organise yourself
NHS will only test vitamins once every 2 years
However GP hasn't tested ferritin, so they should do that for you
While getting vitamin D levels sorted you need to test as minimum annually, but ideally every 6 months
Once you get vitamins optimal and TSH down under 2, possibly lower, with FT4 near top of range, if FT3 remains low then you will need to see endocrinologist to get prescribed small dose of T3
Dionne at Thyroid Uk has list of recommended thyroid specialists who will prescribe T3.
Was total thyroidectomy due to thyroid cancer?
If so your GP is being negligent....TSH should be kept very low
Even without cancer Official NHS guidelines saying TSH should be between 0.2 and 2.0 when on Levothyroxine
(Many of us need TSH nearer 0.2 than 2.0 to feel well)
See box
Thyroxine replacement in primary hypothyroidism
pathology.leedsth.nhs.uk/pa...
No not cancer but thyrotoxicosis twice and bloods didn’t show any problems at first until I was sent to hospital and begged them to do a t3&4 , the result was sky high so they recommended I have it out ASAP. TSH actually stopped working for a while. I did have lots of benign nodules all around thyroid. I have to wait for some results as GP on holiday so maybe ferritin is one of them because I’m sure it was requested.. I got vit D3 capsules on prescription before. I’m hoping this light head will be gone by tomorrow and I have a good sleep tonight.
Thanks.
So you had Graves' disease.
Look at trying strictly gluten free diet
Helps many
While still eating high gluten diet Ideally ask GP for coeliac blood test first or buy test online for under £20, just to rule it out first
Assuming test is negative you can immediately go on strictly gluten free diet
(If test is positive you will need to remain on high gluten diet until endoscopy, maximum 6 weeks wait officially)
Trying gluten free diet for 3-6 months. If no noticeable improvement then reintroduce gluten and see if symptoms get worse
chriskresser.com/the-gluten...
amymyersmd.com/2018/04/3-re...
Hello again Dustpan
Graves is an autoimmune disease and as such it's for life, it's in your blood and your DNA.
There is probably some genetic predisposition, maybe a generation away from you and I read it can be triggered by a sudden shock to the system like having a car accident or hearing of an unexpected death.
Graves antibodies tend to attack the thyroid and for some people also the eyes. The thyroid, is a major important gland, so when under attack the symptoms experienced can be said to be life threatening. In reality the thyroid is not the cause in all this but the victim of an attack from your anti bodies, and simply removing the target of the attack, the thyroid, doesn't actually solve the underlying issue and that of reducing or controlling the Graves antibodies.
It's essential that you are not monitored on TSH blood tests as we can have TSI antibodies sitting on and controlling the TSH giving the impression that we look over medicated when in fact the opposite is probably more likely. it's a bit like having a car, and knowing you need petrol though the dashboard is reading a full tank, because the gauge / TSH is stuck.
I remember recommending one book for you previously, so here are two more giving a lot more in depth knowledge and information than I can offer on this amazing website.
Elaine Moore - Graves Disease a Practical Guide - this lady has the disease and found no help when he went through treatment in the late 1990s, so she wrote this book to help others. There is now a Graves Foundation in her name, it is stateside so medical protocol maybe slightly different but it is well researched, current and much like this platform.
Barbara S Lougheed is another author and researcher of Graves, in the Sates who has the disease. Her book is called Tired Thyroid and I believe she also now runs a " blog ".
It's a massive learning curve, there is much to read and understand.
I am with Graves Disease post RAI 2005 and now self medicating with NDT having been refused a trial of T3 because of my suppressed TSH.
Hi Pennyannie
There are a very few enlightened endocrinologists who will prescribe T3 despite suppressed TSH
But glad to hear you are doing well on NDT
Yes thank you SlowDragon,
Living down here in Cornwall, I feel very much out of the loop - I've tried this county and struck out, the stress and anxiety exacerbating my graves symptoms.
I'm now stress free, confident in my own space and not tied to TSH scores, text book guidelines and being referred to as a conundrum !
So all in all, staying away and thank goodness at this point in time I have no other health issues that necessitate my seeing a doctor.
I trust this site more than any of you will ever know. Thank you one and all.
Just will point out Kernow CCG has by far highest prescription rate for NHS T3 in England
So there must be T3 friendly endocrinologist somewhere!!!
openprescribing.net/analyse...
I know I was shocked when I saw the breakdown.
My surgery shows no T3 or NDT - the surgeries showing NDT are miles out of my catchment area, and having contacted openprescribing, they couldn't give me the doctor's name writing the scripts, as my plan was to write direct to the doctor concerned requesting a private appointment.
Prior to coming on this site, in 2016, I paid to see the head of endocrinology at the one and only hospital we have, and where I had my diagnosis and RAI treatment. He told me he had no problem with me taking T3 or NDT but I would have to buy it myself, and I should go on the web and DIY. That information cost me £185.
I asked about " named patient only prescription " with him and my doctor but they both answered no.
Having been refused T3 in 2018 by an endo in the hospital, I've really had enough with it all. Paying to go private to get a prescription that may or may not be continued by my own doctor and may well cost me a lot more than buying the hormone replacement myself, why would I do that ?
I purchased both T3 and NDT and allowed myself a trial of both. They both did the trick and I found I preferred NDT as it felt softer on my body. Like putting on a pair of slippers compared to T3 feeling like I was wearing high heels two sizes too small.
Maintaining NDT supply and costs seem easier than T3 and being on a single persons pension in a shared ownership property, I have to watch my pennies, so NDT seems to be the most sensible option for me, at this point in time.
I thank you for your concern and information, but maybe I simply look too well or don't interview well or maybe badly enough to qualify for any NHS help.
It's entirely unacceptable for an endocrinologist to advise patients to buy essential medication over the Internet
Hopefully things are slowly moving forward
Well, I know this and find it all totally galling.
Thanks to this site I'm come off the NHS merry go round that was making me more unwell. I feel so disappointed and disillusioned in the NHS, and please don't get me started on giving RAI treatment let alone the consequences that may befall you down the road that no NHS department acknowledges even exist.
Good night SlowDragon - I need to calm down - I'll now try Question Time ????
LOL
Research clearly shows 20% Patients with no thyroid can not regain full health on just Levothyroxine
ncbi.nlm.nih.gov/pmc/articl...
I know, I read this a few days ago, please get with the programme.
We are now talking about who can replace the Prime Minister and if you keep pinging me, I'm going to vote for you xx
We need Honesty, truth and integrity ? yes, you're still in the frame.
At least the threat of being PM has stopped you pinging me xxxxx