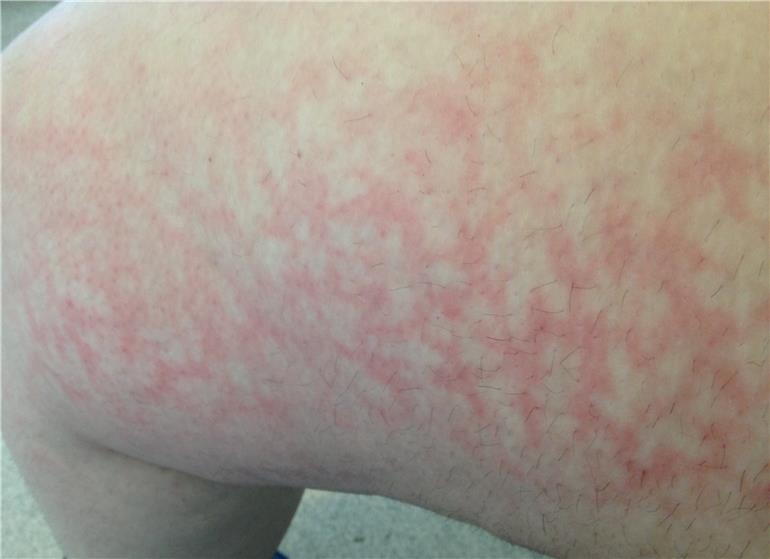
Hi I've been suffering with lupus for 5 years but only got a definite diagnosis a few weeks ago. I suffer a lot with the sun as well as joint pain, sweating, nausea to name but a few! I'm just interested to know if anyone else suffers with a rash like the o e in the picture, i. Was sitting in the sun wiojeans on and my legs started to itch and burn. I also wear compression tights due to another illness so I was well covered.
My lupus skin V the sun: Hi I've been... - LUpus Patients Un...
My lupus skin V the sun
Welcome to LUpus Patients Understanding & Support (LUPUS) at HealthUnlocked.
Rashes are notoriously difficult to diagnose even for a doctor. Have you shown this rash to your rheumatologist or dermatologist? Is this from photosensitivity? Does it irritate?
We also have another website called the LuPUS Message Board where you can also post questions and talk to other people. Registration is FREE and we offer free information and free online psychological support. We specialise in psychological support with our own counsellor/psychotherapist available.
By becoming a Member, you will have access to the private forums and because they are private, only Members have access and even bots and search engines are forbidden.
When you register, please use the following format for entering your date of birth: nn-nn-nnnn where n=number. Please use the "-" separator and not "/".
Finally, please go to: lupus-support.org/LuPUSMB and Sign Up.
I look forward to talking with you more!
Sometimes we need to talk to people who understand and who are not family or friends.
With good wishes!
Ros
Disclaimer: No attempt is made to diagnose or to make any medical judgement. You are advised to seek the advice from your own physician. LUpus Patients Understanding & Support (LUPUS) is not a substitute for your own doctor.
Hi, I've yet to show this rash to my rheumatologist as it's a new one this year. I'm seeing the rheumatologist in a few weeks. Yes it does irritate, it itches and burns and only occurs when I'm in the sun so it is photosensitivity. I have the butterfly rash on my face too and also get the vasculitus rash on my arms and face. I hate summer! Lol I also sweat profusely which of course further irritates the rash😖
The malar rash is a very particular kind of rash. Although it is distinctive for SLE, most lupus patients do not have a malar rash, although they often have other forms of rashes. Many lupus patients are allergic and photosensitive.
I would advise you use the highest SF and use it all the time, even when cloudy. You must wear a hat at all times - a sun hat that prevents the UV rays. You can also buy T-shirts and other kinds of clothes, although I know they are expensive. You can also purchase sun-umbrellas that also prevent the UV rays. Note as well, when driving in a car, you can be badly affected.
From the Lupus Foundation of America
Sun Rules: 5 Facts to Know About Summer Sun Safety
By Emily Wojcik
Now that summer is here, there’s no end to new information about vitamin D, skin cancer, and sun protection factor (SPF) levels. Sun-related topics take on special importance for people with lupus. Here are five facts you need to know for a safer summer.
1. UV rays are not all the same. When we talk about sun exposure, what we really mean is ultraviolet (UV) radiation. The sun emits light at all wavelengths in the electromagnetic spectrum, but ultraviolet rays are the ones responsible for causing skin damage such as sunburns. Ultraviolet rays are divided into three wavelength bands—UVA, UVB, and UVC.
"UVA and UVB are the types that most often penetrate the ozone layer to reach Earth,” says David Fiorentino, M.D., Ph.D., assistant professor of dermatology at the Stanford University School of Medicine. “UVB is shorter—it’s the ‘burning’ ray. It causes sunburn and can damage DNA and cells.”
He cautions, “UVA is longer and can penetrate more deeply into the top layer of the skin—the dermis—which contains the proteins, such as collagen, that make up most of the structure and bulk of our skin.” Both types can cause skin cancer.
UVA can also trigger cutaneous (skin) lupus and cause flares of existing systemic lupus, says Andrew Franks Jr., M.D., a professor of dermatology and medicine and director of the Skin Lupus & Autoimmune Connective Tissue Disease Center at the New York University School of Medicine.
He explains, “UVA rays interfere with the skin’s immunity, allowing damage to cells and promoting the development of autoimmune antibodies, such as ANAs.” ANAs are antinuclear antibodies that bind to a cell’s nucleus, damaging or destroying the cell. Most people with lupus are familiar with the ANA test that helps to confirm a lupus diagnosis by revealing the existence of these damaging autoantibodies. In fact, excessive sun exposure is often the trigger for symptoms that eventually lead to a lupus diagnosis.
Ultraviolet ray levels are not constant: The position of the sun in the sky and low ozone both correlate with increased UV rays. Sand, snow, and water all reflect UV rays. And don’t be fooled by the clouds—they do not block UV. The amounts of UV also vary with altitude, with increased UV penetration at higher altitudes due to the thinner atmosphere.
Skin damage from UV rays also depends on your skin type: Fair skin is less tolerant than dark skin, but all skin types will be affected; it may just take a little longer.
Stacie Collett, 39, of Holly Springs, GA, tells a familiar story. Diagnosed with lupus in 2005, she found that being at the beach caused fatigue and bad headaches, even when she was younger. “In my 20s, I would get this lacy rash on my thighs after being in the sun,” she says. “I thought that was just part of tanning.” Now, she says, “I can’t be in the sun at all. It just zaps my energy.”
2. UV reaction can take many forms. People with lupus need to be aware of UV photosensitivity. “Photosensitivity could mean a systemic response, like feeling sick, having chills, fever, even joint pain, or that you sunburn more easily,” Fiorentino says. Sometimes, though, the reaction may not be visible.
Beth Lindsley, 49, of Three Forks, TX, was diagnosed with lupus three years ago. But she noticed her sensitivity long before that. “I lived in the sun. I coached (high school tennis teams and elementary and middle school kickball teams), surfed, swam, jogged,” she says. “Nine years ago, I started passing out after being in the sun. I would feel shaky and get a little rash. Now I have immediate reactions.” Lindsley’s rheumatologist explained that this type of extreme photosensitivity can cause a flare of lupus, which leads to damage in her internal organs.
“You don’t necessarily know when the damage has been done until it’s too late,” says Franks.
3. There’s no such thing as a “safe” tan from UV light. One of the most dangerous myths about UV rays is that damage occurs only after a sunburn. The idea that a “base tan” will prevent burning and, therefore, prevent illness is particularly troublesome. “Any time you have a tan, it means your skin is trying to protect itself from further damage by producing melanin,” Fiorentino says. While melanin might provide a minimal level of protection, about SPF 6, it also indicates that damage has already been done.
Tanning beds, which use UVA rays, are especially dangerous. “People think tanning parlors are safe because they don’t get burned,” Franks says. “But we now know tanning beds cause a tremendous increase in skin cancer and melanoma.” In fact, Franks notes, 26 states have shut down tanning parlors.
For a tanned look, tanning products are the way to go. Cosmetic bronzers wash off like regular makeup; sunless tanners temporarily stain the skin (see “Protect Your Skin”). But remember: The “tan” you get with these products does not provide UV protection.
4. Vitamin D doesn’t have to come from the sun. For people with lupus, vitamin D is a real concern. “It’s high on everyone’s radar and with good reason,” Fiorentino says. “UVB is required for the body to make vitamin D, so if you use sunscreen or clothing that decreases your UVB exposure, you decrease the vitamin D that your body makes.”
To meet your daily vitamin D requirement without spending extra time in the sunlight, you can eat foods with vitamin D or take vitamin supplements. For most people, the National Institutes of Health recommends 600 international units (IUs) per day, though your doctor may recommend up to 1,000 IUs. “It’s much easier and safer to supplement with vitamins, especially since it’s hard to recommend any sun exposure beyond what people with lupus get in day-to-day life,” Fiorentino says.
5. The right sun protection is more than just SPF. Always be aware of potential sources of UV rays, indoors and out. “Sun is the primary outdoor source of UV light,” says Fiorentino. “Even cloudy days can provide up to 80 percent of the UV of a sunny day.” When indoors and in cars, he says, “the biggest risk is often outdoor sun coming through windows.” While glass does block UVB transmission, most UVA can get through.
Other UV sources can be harder to spot. Franks says the new flat computer and television screens do not emit radiation, but older models do. The bigger concern is lighting. “Halogen and fluorescent lights emit more radiation than incandescent,” he says. “You can, however, completely block UV with plastic covers.” If the bulb is exposed, especially a halogen bulb, “people who are photosensitive can have problems if they are within four feet of it,” Franks says.
Lindsley knows this well. A former teacher, her desk at school was next to a big window and under a large fluorescent light. “All of a sudden I started getting rashes from being near the window,” she says. “I went from wanting every window open to shutting windows and turning the light off. My mom thought I was depressed. She said, ‘You sit in the dark all the time.’”
Today Collett and Lindsley both wear long sleeves and hats and never leave the house without skin protection. Lindsley says, “I coached and taught for 20 years, and lupus took both of those away from me. The one thing it’s not going to take is my participation in life. I’m not going to let it.”
Protect Your Skin
Protective Clothing. Sun-protective clothing, made from specially treated fabrics, is extremely effective, says dermatologist Andrew Franks Jr., M.D. If you want to treat your current clothing, find one of the products that can be added to your laundry to increase fabrics’ SPF from a normal level of about 6 to SPF 15. And when looking for hats, think beyond the baseball cap variety. “You need something with a wider brim, at least four inches all the way around,” Franks says.
Sunscreen or Sunblock? “Sunscreens have an interaction with your skin and absorb UV radiation. Put them on 30 minutes prior to sun exposure to allow your skin to absorb the polymer,” Franks says. Sunblocks, on the other hand, “reflect radiation and immediately block it without a wait time.”
But not all sunblocks protect against both types of UVA rays, UVA-1 and UVA-2. “Right now, by far the best sunscreen on the market today is Mexoryl,™ which blocks both [in addition to UVB],” Franks says. There is more than one brand, so be sure the ingredient list includes Mexoryl. Products with the Helioplex® compound, which Franks says is close to Mexoryl in effectiveness, also protect against UVA-1 and 2. Recommendations from the American Academy of Dermatology are at aad.org.
Eye Protection. Check the labeling: Sun-glasses with at least 99 percent UVA and UVB blockage are the best, especially if they cover the sides of your face, preventing UV rays from entering from the side.
Light Covers. Window film and light shields help protect against UVA and UVB exposure. The Naturalux Light Shields Web site includes a special section on lupus.
DIY Tanning. Find out about self-applied tanning lotions, gels, and sprays at WebMD. (The LFA cannot endorse specific products.)
Editor's Note: On June 15, the Food and Drug Administration (FDA) announced new labeling and product testing guidelines for manufacturers of sunblocks and sunscreens. Click here for more information.
lupus.org/magazine/entry/su...
Here are some websites you may find helpful
You can find more information at the LuPUS Message Board:
I just had some outbreak just like your photo. My upper arms look like lizard skin. I'm undiagnosed for anything specific but ibdid have pos ANA. I go to the VA and my neurologist said I'm fine. Ha!I wish I can post photos. I look like I'm a zombie.
A neurologist is neither a dermatologist, nor a rheumatologist! Ask someone with a mobile/cell phone to take a picture if you can't! A-selfie-of-a-skin-rash!
Although it is true that a diagnosis cannot be made from a photograph, it can help to show you have symptoms. Only a biopsy can confirm the type of rash eg the SLE "malar" rash, which only a minority percentage of patients have! However, there are other rashes which include a V-shaped rash, prickly heat rash or livedo reticularis etc
With good wishes,
Ros
Hi, yes I do I photograph absolutely everything
That's exactly the rash I have had three times now on top of my thigh. I have a photo now too.. Got a lovely collection of photos for my first rheumatologist appt! My rash like that was bright red, fiery. Same shape. Reticulus livedo I believe..
Yes keep photo diary!
Livedo reticularis is thought to be due to spasms of the blood vessels or an abnormality of the circulation near the skin surface. It makes the skin, usually on the legs, look mottled and purplish, in sort of a netlike pattern with distinct borders.
Livedo reticularis is a livedoid discolouration of the skin in a reticular pattern. Broadly speaking, livedo is divided into physiological and pathological livedo. Physiological livedo (cutis marmorata) is commonly seen on the legs of infants and young women in cold weather and improves on rewarming. Pathological livedo is a cutaneous manifestation of a number of systemic conditions, most notably the Antiphospholipid syndrome (APS), and is associated with arterial and venous thrombosis and increased pregnancy morbidity irrespective of the presence of antiphospholipid antibodies.
Pathological livedo reticularis may be a sign of vasculitis or of obstruction of the vessel by a circulating material. Causes include the following:
Livedo can be an initial manifestation in the primary APS, and up to 70% of patients with systemic lupus erythematosus associated with the APS
Polyarteritis nodosa and antineutrophil cytoplasmic antibody (ANCA)-positive vasculitis
Cryoglobulinaemia
Other connective tissue disorders such as dermatomyositis and rheumatoid arthritis
Thromboangiitis obliterans
Primary thrombocytopenia and polycythaemia vera
Pyoderma gangrenosum
Sneddon's syndrome is a form of idiopathic livedo reticularis with systemic involvement ie internal blood vessels are affected, most commonly in the brain, eye and heart
Clinical findings
Classical cutaneous features of livedo reticularis
A red-blue, reticular (net-like) discolouration surrounding pale central areas
The network may comprise regular unbroken circles or an irregular broken pattern
It occurs mostly on the legs, arms and trunk and is more pronounced in cold weather
In physiological livedo the signs improve as the skin warms, and the patient is otherwise well
In pathological livedo the rash is persistent, non-reversible with rewarming, and the patient may be unwell
The term livedo racemosa is sometimes used when the livedo is more generalised, and has an irregular-broken shape. While this pattern is recognised in Sneddon's syndrome, it can also be found in other causes of pathological livedo such as the APS and the ANCA-positive vasculitides
Livedoid vasculopathy
Livedo may present as a cutaneous ulcer (livedoid vasculopathy), and atrophie blanche may be a consequence
It usually affects the lower legs bilaterally and is more common in summer
It may affect all age groups but is more common in young females
Initially there is a painful papular rash that develops into an ulcer. The ulcer subsequently heals leaving a porcelain white scar (atrophie blanche) that is often star-shaped
Livedoid vasculopathy was originally described as a clinical manifestation of vasculitis; however the present concept is that it is a vaso-occlusive phenomenon with thrombosis of intradermal venules. It may be primary, or secondary, for example to a coagulopathy such as the APS or cryoglobulinaemia
Systemic associations with pathological livedo reticularis
Arterial and venous thrombosis has been observed in patients with livedo irrespective of the presence of antiphospholipid antibodies
Pregnancy morbidity also appears to be higher in patients with SLE and livedo, even when negative for antiphospholipid antibodies
Accelerated atherosclerosis may be a feature
I photograph everything lol
I think you have Livedo reticularis caused by Hughes Syndrome. Please get tested for it.
Good luck!
Thankyou, I will x
From what I understand, the UV rays with us Lupus people,dose'nt just stop at the first 2 derma layers when some have 'sunburn', with us it keeps going right down to even level 6,to the internal organs! What's happening here is that the jeans and compression devices you were wearing 'drew down' the UV rays well below the surface of the textiles and caused damage deep inside your legs? Just because it's 'thick' doesn't mean it offers 'any' UV protection, unless those clothes were treated entirely with a anti-uva/uvb specific treatment spray, as they will ALWAYS cause damage when worn outside in the sunshine! Conversely, just because it's 'light and white' also dose not mean you or I get more than about 3-5 mins protection in this heat?
You now know you are to stay out of the sun at all times? Even just to put the rubbish out wear sunglasses and cover up your head with hat, get into a routine quickly. Wear, in your case either UV protection clothing 'full length' or 'cover yourself full length' with factor 50 sun block,from the feet up especially if wearing summer shoes/sandles. Regularly reapplying in accordance with the manufacturers guidance. You can get this on prescription.
I learnt really quick after my first full-ln flare at Easter brought on by simply 'hanging out a my washing on the line before 9am' in all of about 4 mins? That made my arms look like boiled water was poured over them later that day,the angry butterfly appeared, the indescribable agony of the inflammatory arthritis that came with the Lupus that prevented me from walking as it and the lupus attacked all the supporting soft tissues of both a knees and destabalized them, kept me from sleeping for 2 weeks flat, the sweats,the head aches,the rye pain,the lack of appetite, the 'mottled rash' all over the rest of the body (that gradually faded after a week) that I had a choice- either get serious about this and educate myself as fast as possible off the web or have another 3 months from hell?
Now I wear huge hats, big shawls, wrap around sunglasses in amber lenses (that stopped the headaches and eye pains) a sun umbrella ,'salwar kameez' in this heat with 'extra long sleeves' bespoke made, maxi dresses, always covering up my arms with big shirts/jackets ,fingerless multilayer gloves ect, but before everything, I cover EVERYWHERE I can reach paying especial attention to the ears, neck ,nape, nose-tip,lips ect with uva/uvb factor 50!
I've recently found out I have an issue with uvb so I have to have this specifically on my face (and all down my right drivers side in addition to a 10 hour one underneath) or in the first rays of the rising sun I go like a beetroot!
Have you also found that Stores lighting effects you, even to the point that it changes from store to store in 'any' of the chains? I found that same super market chain in one store I could only tollerate 1 hour because of new flashy lighting and no protection on Windows so started to feel ill fairly quickly? Another branch I could do 2 hours because they hadn't had the 'up grade' and had protective film on all glass windows ect.
Hi Jokelby72,
I hope you don’t mind me asking if you ever found out if your rash was related to lupus. I have a rash that looks exactlyyy like yours (I was bad and was in the sun a bit yesterday) and it has been accompanied by flaring my other symptoms.
Hope you are well!
I have this exactly but no diagnosis.
Hi Jokelby72
I found your picture today and this is the exact same rash that appeared on my legs after sitting outside in the sunshine. I was wearing Jeans. I have been diagnosed with Primary Lymphoedema so I usually wear 30mg compression stockings on both legs every day too.
Interested in the fact that you mentioned you also wear compression tights due to another illness. Is it Lymphoedema?
Hello, I just discovered this forum & signed up to reply to your post. I’ve been diagnosed with fibromyalgia, Raynauds (primary) & UCTD (undifferentiated connective tissue disease) with a positive ANA. I realize everyone replying is focusing on the sun as the cause & photosensitivity being the culprit, but I disagree completely.
I too have sun sensitivity, where I get a rash/burn similar to malar, but more like raccoon (never my nose or chin) & the front/sides of my neck. Sometimes the burns are so bad I’ve gotten blisters, but the skin always peels off in layers (not at all like a bad sunburn but more like skin peeling from a bad abrasion, like road rash from falling off your bike).
I also however get this bright red lacy netting-type rash on my legs and arms, but I don’t believe it’s from UV exposure, it’s from the *heat*. When I first started getting these rashes, it was from being in the sauna, not the sun. It happens when I’m outside as well, but it’s from the heat, not the UV exposure. It only happens when the heat gets intense (only when I’m sitting in the heat, not if I’m walking around).
The dermatologist I waited for months to see gave me no answers. My rash doesn’t actually hurt or itch like others have mentioned. It usually goes away within 30 minutes & leaves no lasting marks.
It does look just like the photos I’ve seen online of livedo reticularis. The part that confuses me is mine is definitely only caused by heat. It says livedo reticularis is caused by cold & resolves with heat.
I’m aware my post doesn’t solve anything, but I’m curious if others are really triggering this lacy rash by *heat* and not UV rays?
I get a flushing rash on my cheeks from heat. The rashes I get from the sun are different. I also have UCTD. Could the sauna be causing vasodilation? That is what heat does to me. Can you post a photo?
Hi. I get a burning rash (painful & lasts for up to a week) on my face from the sun but the lacy (pain free) red rash from the heat (on my extremities) resolves very quickly.
I have a couple photos I took last month of the lacy rash that I can upload but I’ll have to get the face rash photos from my computer & can upload those later.
I just need to figure out how to upload photos... 
Good. Mine is gone by the next day.
That’s good yours resolves fast. I can’t find a way to post a photo to an existing thread. I see it as an option for a new post, but can’t figure it out here. Can you tell me how to upload to this string?
Just coming across this in search of my own answers for my legs doing the same thing with jeans on. I have multiple autoimmune diseases and just tested today for lupus.
I get a rash like this after any sun exposure. Even if it’s driving in the car and the sun hits my legs or arms. I have SLE.